Stress Levels of Nurses in Oncology Outpatient Units
Background: Oncology nursing is often a source of substantial stress for nurses. Many nurses, particularly novice nurses, have inadequate preparation to care for patients at the end of life and their families. Unless nurses prevent or manage work-related stress by using effective coping strategies, oncology nursing staff will continue to suffer from burnout and compassion fatigue.
Objectives: The purpose of this article is to identify stress levels and stressful factors of nurses working in oncology outpatient units and to explore coping behaviors for work-related stress of oncology staff nurses in outpatient units.
Methods: A descriptive, cross-sectional design was used to identify stress levels and stressful factors for outpatient oncology nurses, investigate differences in stress levels among nurses’ demographic characteristics, and explore coping behaviors of the nurses. Study participants (N = 40) included RNs and licensed practical nurses who completed the Nursing Stress Scale, three open-ended questions, and a demographic questionnaire.
Findings: The highest sources of stress were workload and patient death and dying. Demographic variables of age and work experience in nursing showed a significant positive relationship to work-related stress scores. The three most frequently used coping behaviors were verbalizing, exercising or relaxing, and taking time for self. Continuing education programs on stress management are highly recommended. Outpatient oncology nurses should be nurtured and supported through tailored interventions at multiple levels to help them find effective coping strategies and develop self-care competencies. Although younger and less experienced nurses had lower mean stress scores than older and more experienced nurses, the continuing education programs and tailored interventions would be helpful for all oncology nursing staff.
Jump to a section
The specialty of oncology nursing is often a source of much stress for nurses (Escot, Artero, Gandubert, Boulenger, & Ritchie, 2001; Rodrigues & Chaves, 2008). The stress stems from high exposure to various trying situations specific to the oncology workplace, such as complex cancer treatments and patient deaths (de Carvalho, Muller, de Carvalho, & de Souza Melo, 2005). In addition, most nurses, particularly novice nurses, have inadequate preparation to care for patients at the end of life and their families (Caton & Klemm, 2006; Gallagher & Gormley, 2009). Accordingly, nursing staff working in oncology units are vulnerable to stress at work (de Carvalho et al., 2005; Ergün, Oran, & Bender, 2005).
In addition to stressful situations in work settings, oncology nurses frequently ignore or neglect their emotional experiences when caring for patients with cancer (Boyle, 2000; Bush, 2009; Medland, Howard-Ruben, & Whitaker, 2004). This may come from unawareness of the link between work and their own health (Medland et al., 2004; Sabo, 2008) or prolonged exposure to work stressors (Bush, 2009). This lack of perception of their own health leads to ineffective coping behaviors and negative emotions, such as feelings of failure, continuous pressure, and depression (Conte, 2011; Escot et al., 2001). Unless nurses prevent or manage work-related stress by using effective coping strategies, oncology nursing staff will continue to suffer from burnout and compassion fatigue (Aycock & Boyle, 2009; Bush, 2009). Nurses who do not deal with stress effectively also may leave the oncology workplace and, potentially, the nursing profession (Conte, 2011; Medland et al., 2004). Consequently, practical interventions are needed to help nurses better manage stress in the workplace and remain in oncology settings.
Although all facets of oncology nursing may be stressful (Davis, Lind, & Sorensen, 2013; Medland et al., 2004), most previous oncology nursing studies on stress and coping have concentrated on care occurring in inpatient settings. Additional work-related stress research for nurses working in outpatient oncology settings is necessary. The process of assessing stress levels and stressful factors is imperative for outpatient oncology nurses and their employers to understand the importance of nurses’ mental health and the existence of stressful factors in oncology settings. This article describes stress levels of oncology nurses in outpatient units, specific stressful factors for nurses in the workplace, differences in stress levels among nurses’ demographic characteristics (e.g., age, marital status, education levels, work experience in nursing), and nurses’ coping behaviors for managing occupational stress.
Literature Review
Stressful Factors in Oncology Nursing
Oncology nursing services are performed in stressful work environments to meet the special needs of patients with cancer and their families (de Carvalho et al., 2005; Ergün et al., 2005). Stressful factors in the oncology specialty commonly include relationships with other medical team members, increased patient acuity, insufficient workplace training, and lack of time for end-of-life care (Ergün et al., 2005; Escot et al., 2001). In addition, the grief and loss experience of oncology nurses can cause long-term stress because of unresolved cumulative grief and loss (Conte, 2011). Brown and Wood (2009) showed that oncology nursing staff members had a tendency to avoid expressing their emotions. Many nurses working with patients with cancer also suppress feelings of grief in their workplaces (Boyle, 2000; Medland et al., 2004). de Carvalho et al. (2005) investigated arduous work situations of nursing staff members caring for adult and pediatric patients with cancer. Situations identified as being most stressful were making mistakes, lacking support from hospital administrators for improving working conditions, lacking equipment and supplies, feeling powerless or helpless, and watching suffering patients with no alternative treatment.
Work-Related Stress Responses
Specific demographic characteristics place nurses at high risk for occupational stress (Isikhan, Comez, & Danis, 2004; Quattrin et al., 2006). According to Isikhan et al. (2004), staff members in oncology settings who had greater work stress scores were employed as nurses, were married, were aged 21–36 years, and had oncology work experience of 1–10 years. Three studies found that oncology nursing staff members with higher scores of emotional exhaustion were aged older than 40 years, were outpatient RNs, had advanced degrees, and had work experience of more than 15 years in oncology (Davis et al., 2013; Potter et al., 2010; Quattrin et al., 2006).
Work-related stress for oncology nurses appears in diverse forms, negatively affecting physical, mental, and psychosocial health (Aycock & Boyle, 2009; Escot et al., 2001). Stress-related health problems include headache, backache, excessive nervousness, sleep disturbances, feelings of continuous stress, and inability to seek pleasant activities in everyday life (Aycock & Boyle, 2009; Escot et al., 2001; Isikhan et al., 2004). In addition, with unresolved grief, nurses can have acute (e.g., anger, anxiety, guilt) or chronic ongoing mental health problems (e.g., burnout, grief, compassion fatigue) (Hildebrandt, 2012). According to Bush (2009) and Potter et al. (2010), oncology nursing staff members are particularly prone to burnout and compassion fatigue by repeated exposure to patients’ distress, death of patients, and care of patients’ families.
Coping Strategies for Occupational Stress
Ekedahl and Wengström (2006) classified coping strategies of nurses caring for patients with cancer into two groups: functional and dysfunctional patterns. Functional coping patterns included creating boundaries at individual (e.g., separating working hours and spare time), group (e.g., developing new routine tasks in oncology units), and institutional levels (e.g., seeking places outside work for relaxation, receiving support from patients or friends, having fun with coworkers, using humor at work). Conversely, lack of boundaries and colleagues’ support contributed to dysfunctional coping patterns that negatively influenced nurses’ health (e.g., increased blood pressure). In addition, oncology nurses used other coping methods for their occupational stress: positive reevaluation (emotion-focused coping), problem solving (problem-focused coping) (Rodrigues & Chaves, 2008), self-confident manner, social support, and optimistic attitude (Isikhan et al., 2004).
Because of the vulnerability of oncology staff members to work-related stress, healthcare professionals must reduce or prevent stress at work and maintain and support optimal wellness conditions. Investigating stress levels, specific stressors, and coping behaviors among oncology nurses in outpatient settings is the first stage of developing tailored interventions and providing supportive work environments for stress management.
Methods
Study approval was received from the institutional review boards of North Dakota State University and Sanford Health, both in Fargo, North Dakota. The current study was conducted at Sanford Roger Maris Cancer Center, which is part of Sanford Health and offers outpatient services to adult and pediatric patients with cancer in four oncology units. Forty oncology nurses working in the four outpatient units were recruited from the nurses’ monthly unit meetings or by mail. Participants completed the Nursing Stress Scale (NSS), three open-ended questions, and a demographic questionnaire. For nurses not attending a unit meeting, respondents returned the completed surveys to the researchers by mail in sealed, self-addressed, stamped envelopes.
The NSS, developed by Gray-Toft and Anderson (1981) was used to measure levels of stress frequency and stressful factors. The NSS consists of seven subscales regarding different sources of stress. A total of 34 items are divided into seven subscales: patient death and dying (seven items), conflict with physicians (five items), inadequate preparation (three items), lack of support (three items), conflict with other nurses (five items), workload (six items), and uncertainty concerning treatment (five items). Each item has a four-point scale ranging from 1 (never) to 4 (very frequently), with higher scores indicating greater levels of stress. Scores on the NSS are summed for a total stress score ranging from 34–136. The test-retest reliability coefficient for the total scale was 0.81, and the internal consistency coefficients ranged from 0.79–0.89. Three open-ended questions were developed based on review of the literature to explore coping behaviors, resources available at work, and additional resources for occupational stress. The demographic questionnaire also was developed by the researchers to investigate differences in stress levels among nurses’ demographic variables.
Data were analyzed using descriptive statistical analyses. All 34 NSS item responses were calculated for each participant and classified into one of three different levels of stress: no stress or less stress (total score of 70 or less), moderate stress (total score of 71–90), or high stress (total score of 91–110). The mean scores of the seven subcategories of the NSS were calculated after obtaining the total subcategory scores. One-way analysis of variance (ANOVA) using SAS®, version 9.3, was performed to test whether stress levels differed among the variables for age, nursing experience, and oncology nursing experience. T-test using pooled (equal) variances was used to examine whether stress levels of participants differed among the variables of marital status and education level. Content analysis was performed on the qualitative data obtained from the three open-ended questions.
Results
Surveys were distributed to 78 nurses, and 40 were returned for a response rate of 51.3%. Demographic data revealed that all were female, 16 were aged 20–30 years, 32 were married, 28 were RNs with a bachelor of science in nursing degree, and 12 had more than 20 years of experience in nursing. Most respondents had worked in oncology for as many as five years or from 6–10 years (see Table 1).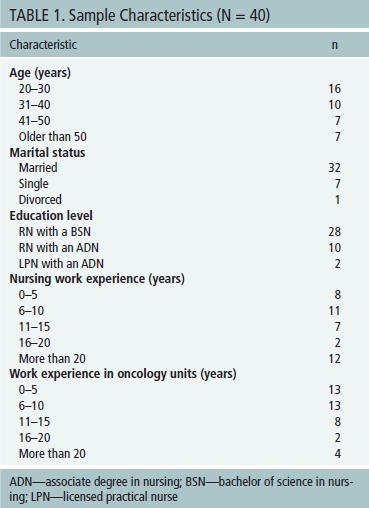 
In the current study, total scores of the NSS ranged from 51–92, with a mean score of 71.35 (SD = 9.43). The NSS total scores were classified into three levels of stress: 18 were considered to be no stress or less stressed, 21 were regarded as moderately stressed, and 1 was considered to be highly stressed. The two most stressful factors were workload and patient death and dying. Inadequate preparation and lack of support were identified as the least stressful factors (see Table 2). 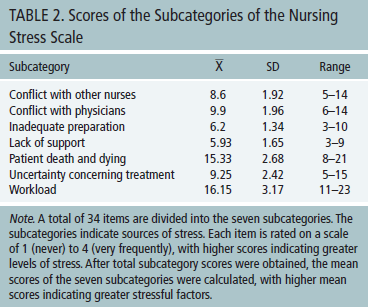
Among five demographic characteristics, participants who had higher mean stress scores were aged from 41–50 years, were married, were RNs with an associate degree in nursing, had work experience in nursing for 11–15 years, and had work experience in oncology for 11–15 years. The means and standard deviations are presented in Table 3. The two variables of age and work experience in nursing had a significant effect on work-related stress scores. Other variables of marital status, education level, and work experience in oncology units showed no significant differences on stress levels (p > 0.05). All respondents were female, eliminating the gender variable. 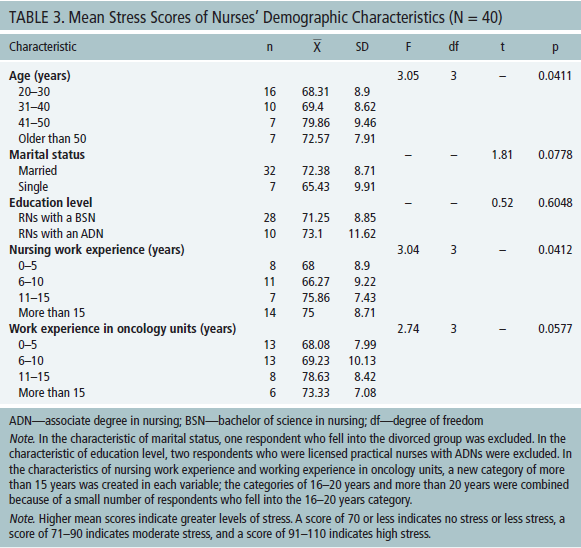
Apart from the NSS, participants were asked to write responses to three open-ended questions concerning occupational stress. The first open-ended question was, “How would you describe your coping behavior to manage work-related stress?” The three most frequently used coping behaviors to relieve occupational stress were verbalizing, exercising or relaxing, and taking time for self (see Table 4). 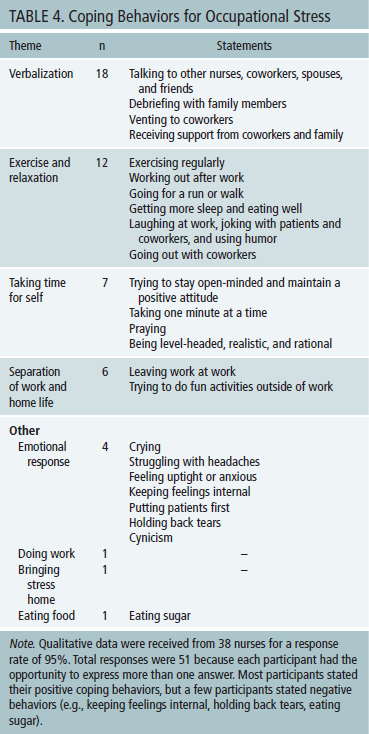
Discussion
Results of the current study revealed that more than half of the respondents reported being moderately stressed. Overall, the results suggest that the outpatient oncology nurses in the current study experienced a moderate degree of work-related stress. Given these data, occupational stress needs to be managed to prevent nurses from becoming highly stressed and to assist them in transitioning to no stress or less stress.
Findings that the highest sources of stress were workload and patient death and dying are supported by previous research. Rodrigues and Chaves (2008) identified the most stressful situations for oncology nurses as patient death, emergency work situations, relationships among team members, and work process factors. According to Rodrigues and Chaves (2008), work process factors included arguments about behaviors of workers that were not accepted by other team members and how work shifts were determined. In the current study, an additional possible stress factor was relationship with professional coworkers, combining the two subscales of conflict with physicians and conflict with other nurses. Because the combined subscales had the highest mean stress score (mean = 18.5), it could be viewed as the most important factor for nurses. In other studies, having relationship difficulties with coworkers was reported as contributing to work-related stress in oncology nurses (Escot et al., 2001; Isikhan et al., 2004).
One-way ANOVA is a reasonable method to analyze data for the NSS, which is a validated, reliable instrument. Because mean stress scores for the variables of age and work experience in nursing were statistically significant, one could ask whether the difference in stress scores was clinically important. The differences are anticipated to be clinically important, but additional research projects would be needed for verification.
An interesting finding of the age variable correlating with occupational stress scores (p < 0.05) was that older participants aged from 41–50 years had a greater mean stress score than participants aged from 20–30 years. These results were inconsistent with a study by Isikhan et al. (2004) using the Job Stress Inventory for oncology nurses and oncologists. Isikhan et al. (2004) found that participants aged from 21–36 years had a higher mean stress score (mean = 31.59) than participants aged 36 years or older (mean = 29.47) (p < 0.05). However, the current study was similar to two previous studies. Potter et al. (2010) reported that healthcare providers with 11–20 years of oncology experience were at greatest risk for burnout and compassion fatigue, and Quattrin et al. (2006) reported that oncology nurses with more than 15 years of oncology experience had higher levels of emotional exhaustion. Additional research in this area is needed to verify the relationship among stress levels, age, and work experience using the same research instruments and populations.
Apart from nurses’ demographic variables, the type of oncology work setting can be a crucial factor in the level of burnout among oncology nurses. Potter et al. (2010) found that inpatient oncology staff members had a higher percentage of high-risk burnout scores (44%) than outpatient staff (33%), but the results were not statistically significant. However, Davis et al. (2013) noted that emotional exhaustion was significantly higher for RNs working in the outpatient setting than for those in the inpatient setting. Because of mixed results, additional research is needed to identify the relationship between the level of burnout and work setting characteristics.
[[{"type":"media","view_mode":"media_original","fid":"22446","field_deltas":{},"link_text":null,"attributes":{"height":"481","width":"368","class":"media-image media-element file-media-original","data-delta":"1"},"fields":{}}]]
Current results of coping behaviors for occupational stress were consistent with findings by Ekedahl and Wengström (2006), who indicated that oncology nurses used coping strategies of making boundaries, venting emotions, receiving support from colleagues, and humor. Data regarding resources available at work to help nurses manage stress were gained from the second open-ended question, “What resources has your workplace made available to help manage work-related stress?” Many participants stated that chaplain services and managers were available to relieve their stress (see Table 5). Information about additional resources at the organizational level for nurses’ job-related stress was collected from the third open-ended question, “What would help you to improve your management of work-related stress?” (see Table 6). Two major requested resources were related to the issues of staffing level and nursing management support. 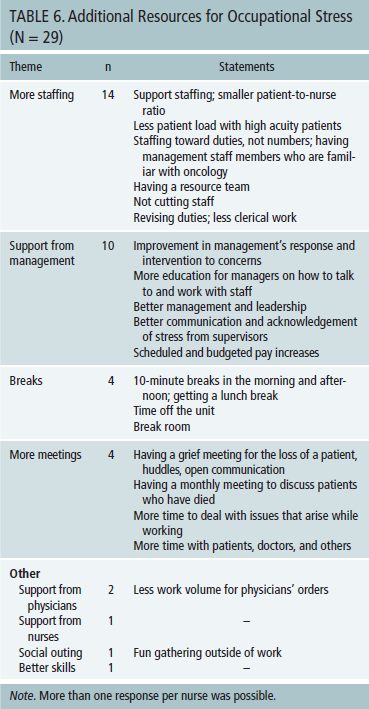
Limitations
The current study was conducted in only one outpatient oncology setting in a medical center. Although the return rate was higher than average, a sample size of 40 limits generalizability of findings to other oncology nursing settings. The current study also was limited to measuring stress frequency levels and sources; the researchers did not measure the intensity of stress for participants. Additional research is needed to more precisely measure intensity of occupational stress for this target population by modifying the NSS or developing a new nursing stress instrument.
Implications for Practice
The current study has clinical implications for developing interventions to help nurses decrease stress levels. Nurse educators and leaders should develop interventions (e.g., exercise and support groups, counseling resources, stress management classes), encourage verbalization of feelings, and encourage expression of grief to assist nurses in effectively managing their stress (Aycock & Boyle, 2009; Henry, 2014; Medland et al., 2004).
Health institutions should consider establishing more supportive work environments and developing interventions tailored to the specific stressors of nurses. In the current study, participant responses identified workload and patient death and dying as the most stressful factors. In response to comments from participants, several interventions at an institutional level (e.g., increasing staff, offering additional unit supervisor support, providing more breaks) could be used to improve stress levels (Henry, 2014; Traeger et al., 2013).
Customized intervention strategies for oncology nurses aged from 41–50 years would be helpful because that age group had the greatest stress score. Stress levels reported by the nurses could have been affected by personal life stressors, which are factors external to the work environment. Nurses with dual responsibilities could have extra sources of stress that negatively influence emotional and physical health and aggravate levels of work-related stress. Interventions could include problem solving; clinical ladder programs; staff recognition; art, music, and pet therapies for staff; self-care; social support; on-site counselors; normalization of experiences; and positive reappraisal (Henry, 2014; Parikh, Taukari, & Bhattacharya, 2004; Potter et al., 2013).
Conclusion
Oncology nurses frequently experience various stressful situations in the workplace that can lead to physical, mental, and psychosocial health problems. Nurses must be able to care for themselves to maintain their optimal health conditions and to reduce or prevent stress at work. Important actions are recognizing adverse effects of work-related stress on health and acknowledging nurses’ emotional experiences. Based on the results of the current study, outpatient oncology nurses should be nurtured and supported through tailored interventions at multiple levels for finding effective coping strategies and developing self-care competencies. By using these interventions, nurses can control their stress, become more satisfied, and improve life quality. Therefore, the quality of patient care and the retention of nursing staff likely will improve.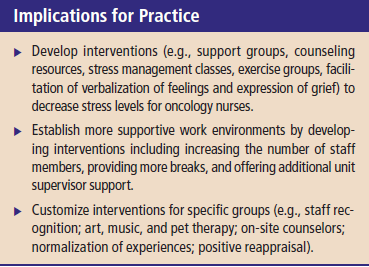 
References
Aycock, N., & Boyle, D. (2009). Interventions to manage compassion fatigue in oncology nursing. Clinical Journal of Oncology Nursing, 13, 183–191. doi:10.1188/09.CJON.183-191
Boyle, D.A. (2000). Pathos in practice: Exploring the affective domain of oncology nursing. Oncology Nursing Forum, 27, 915–919.
Brown, C., & Wood, A. (2009). Oncology nurses’ grief: A literature review. Clinical Journal of Oncology Nursing, 13, 625–627. doi:10.1188/09.CJON.625-627
Bush, N.J. (2009). Compassion fatigue: Are you at risk? Oncology Nursing Forum, 36, 24–28. doi:10.1188/09.ONF.24-28
Caton, A.P., & Klemm, P. (2006). Introduction of novice oncology nurses to end-of-life care. Clinical Journal of Oncology Nursing, 10, 604–608. doi:10.1188/06.CJON.604-608
Conte, T.M. (2011). Pediatric oncology nurse and grief education: A telephone survey. Journal of Pediatric Oncology Nursing, 28, 93–99. doi:10.1177/1043454210377900
Davis, S., Lind, B.K., & Sorensen, C. (2013). A comparison of burnout among oncology nurses working in adult and pediatric inpatient and outpatient settings [Online exclusive]. Oncology Nursing Forum, 40, E303–E311. doi:10.1188/13.ONF.E303-E311
de Carvalho, E.C., Muller, M., de Carvalho, P.B., & de Souza Melo, A. (2005). Stress in the professional practice of oncology nurses. Cancer Nursing, 28, 187–192. doi:10.1097/00002820-200505000-00004
Ekedahl, M., & Wengström, Y. (2006). Nurses in cancer care—Coping strategies when encountering existential issues. European Journal of Oncology Nursing, 10, 128–139. doi:10.1016/j.ejon.2005.05.003
Ergün, F.S., Oran, N.T., & Bender, C.M. (2005). Quality of life of oncology nurses. Cancer Nursing, 28, 193–199.
Escot, C., Artero, S., Gandubert, C., Boulenger, J.P., & Ritchie, K. (2001). Stress levels in nursing staff working in oncology. Stress and Health, 17, 273–279. doi:10.1002/smi.907
Gallagher, R., & Gormley, D.K. (2009). Perceptions of stress, burnout, and support systems in pediatric bone marrow transplantation nursing. Clinical Journal of Oncology Nursing, 13, 681–685. doi:10.1188/09.CJON.681-685
Gray-Toft, P., & Anderson, J.G. (1981). The Nursing Stress Scale: Development of an instrument. Journal of Behavioral Assessment, 3, 11–23. doi:10.1007/BF01321348
Henry, B.J. (2014). Nursing burnout interventions: What is being done? Clinical Journal of Oncology Nursing, 18, 211–214. doi:10.1188/14.CJON.211-214
Hildebrandt, L. (2012). Providing grief resolution as an oncology nurse retention strategy. Clinical Journal of Oncology Nursing, 16, 601–606. doi:10.1188/12.CJON.601-606
Isikhan, V., Comez, T., & Danis, M.Z. (2004). Job stress and coping strategies in health care professionals working with cancer patients. European Journal of Oncology Nursing, 8, 234–244. doi:10.1016/j.ejon.2003.11.004
Medland, J., Howard-Ruben, J., & Whitaker, E. (2004). Fostering psychosocial wellness in oncology nurses: Addressing burnout and social support in the workplace. Oncology Nursing Forum, 31, 47–54. doi:10.1188/04.ONF.47-54
Parikh, P., Taukari, A., & Bhattacharya, T. (2004). Occupational stress and coping among nurses. Journal of Health Management, 6, 115–127. doi:10.1177/097206340400600204
Potter, P., Deshields, T., Berger, J.A., Clarke, M., Olsen, S., & Chen, L. (2013). Evaluation of a compassion fatigue resiliency program for oncology nurses. Oncology Nursing Forum, 40, 180–187. doi:10.1188/13.ONF.180-187
Potter, P., Deshields, T., Divanbeigi, J., Berger, J., Cipriano, D., Norris, L., & Olsen, S. (2010). Compassion fatigue and burnout [Online exclusive]. Clinical Journal of Oncology Nursing, 14, E56–E62. doi:10.1188/10.CJON.E56-E62
Quattrin, R., Zanini, A., Nascig, E., Annunziata, M.A., Calligaris, L., & Brusaferro, S. (2006). Level of burnout among nurses working in oncology in an Italian region. Oncology Nursing Forum, 33, 815–820. doi:10.1188/06.ONF.815-820
Rodrigues, A.B., & Chaves, E.C. (2008). Stressing factors and coping strategies used by oncology nurses. Revista Latino-Americana de Enfermagem, 16, 24–28.
Sabo, B.M. (2008). Adverse psychosocial consequences: Compassion fatigue, burnout and vicarious traumatization: Are nurses who provide palliative and hematological cancer care vulnerable? Indian Journal of Palliative Care, 14, 23–29.
Traeger, L., Park, E.R., Sporn, N., Repper-DeLisi, J., Convery, M.S., Jacobo, M., & Pirl, W.F. (2013). Development and evaluation of targeted psychological skills training for oncology nurses in managing stressful patient and family encounters [Online exclusive]. Oncology Nursing Forum, 40, E327–E336.
[[{"type":"media","view_mode":"media_original","fid":"22501","field_deltas":{},"link_text":null,"attributes":{"height":"192","width":"764","class":"media-image media-element file-media-original","data-delta":"2"},"fields":{}}]]
About the Author(s)
Woonhwa Ko, MS, RN, recently graduated from the Master of Science Nurse Educator Program and Norma Kiser-Larson, PhD, RN, is an associate professor and the Master of Science Nurse Educator Program Director, both in the Department of Nursing at North Dakota State University in Fargo. The authors take full responsibility for the content of the article. The authors did not receive honoraria for this work. The content of this article has been reviewed by independent peer reviewers to ensure that it is balanced, objective, and free from commercial bias. No financial relationships relevant to the content of this article have been disclosed by the authors, planners, independent peer reviewers, or editorial staff. Ko can be reached at hwa9401@yahoo.com, with copy to editor at CJONEditor@ons.org. (Submitted June 2014. Revision submitted May 2015. Accepted for publication May 21, 2015.)
References
Aycock, N., & Boyle, D. (2009). Interventions to manage compassion fatigue in oncology nursing. Clinical Journal of Oncology Nursing, 13, 183–191. doi:10.1188/09.CJON.183-191
Boyle, D.A. (2000). Pathos in practice: Exploring the affective domain of oncology nursing. Oncology Nursing Forum, 27, 915–919.
Brown, C., & Wood, A. (2009). Oncology nurses’ grief: A literature review. Clinical Journal of Oncology Nursing, 13, 625–627. doi:10.1188/09.CJON.625-627
Bush, N.J. (2009). Compassion fatigue: Are you at risk? Oncology Nursing Forum, 36, 24–28. doi:10.1188/09.ONF.24-28
Caton, A.P., & Klemm, P. (2006). Introduction of novice oncology nurses to end-of-life care. Clinical Journal of Oncology Nursing, 10, 604–608. doi:10.1188/06.CJON.604-608
Conte, T.M. (2011). Pediatric oncology nurse and grief education: A telephone survey. Journal of Pediatric Oncology Nursing, 28, 93–99. doi:10.1177/1043454210377900
Davis, S., Lind, B.K., & Sorensen, C. (2013). A comparison of burnout among oncology nurses working in adult and pediatric inpatient and outpatient settings [Online exclusive]. Oncology Nursing Forum, 40, E303–E311. doi:10.1188/13.ONF.E303-E311
de Carvalho, E.C., Muller, M., de Carvalho, P.B., & de Souza Melo, A. (2005). Stress in the professional practice of oncology nurses. Cancer Nursing, 28, 187–192. doi:10.1097/00002820-200505000-00004
Ekedahl, M., & Wengström, Y. (2006). Nurses in cancer care—Coping strategies when encountering existential issues. European Journal of Oncology Nursing, 10, 128–139. doi:10.1016/j.ejon.2005.05.003
Ergün, F.S., Oran, N.T., & Bender, C.M. (2005). Quality of life of oncology nurses. Cancer Nursing, 28, 193–199.
Escot, C., Artero, S., Gandubert, C., Boulenger, J.P., & Ritchie, K. (2001). Stress levels in nursing staff working in oncology. Stress and Health, 17, 273–279. doi:10.1002/smi.907
Gallagher, R., & Gormley, D.K. (2009). Perceptions of stress, burnout, and support systems in pediatric bone marrow transplantation nursing. Clinical Journal of Oncology Nursing, 13, 681–685. doi:10.1188/09.CJON.681-685
Gray-Toft, P., & Anderson, J.G. (1981). The Nursing Stress Scale: Development of an instrument. Journal of Behavioral Assessment, 3, 11–23. doi:10.1007/BF01321348
Henry, B.J. (2014). Nursing burnout interventions: What is being done? Clinical Journal of Oncology Nursing, 18, 211–214. doi:10.1188/14.CJON.211-214
Hildebrandt, L. (2012). Providing grief resolution as an oncology nurse retention strategy. Clinical Journal of Oncology Nursing, 16, 601–606. doi:10.1188/12.CJON.601-606
Isikhan, V., Comez, T., & Danis, M.Z. (2004). Job stress and coping strategies in health care professionals working with cancer patients. European Journal of Oncology Nursing, 8, 234–244. doi:10.1016/j.ejon.2003.11.004
Medland, J., Howard-Ruben, J., & Whitaker, E. (2004). Fostering psychosocial wellness in oncology nurses: Addressing burnout and social support in the workplace. Oncology Nursing Forum, 31, 47–54. doi:10.1188/04.ONF.47-54
Parikh, P., Taukari, A., & Bhattacharya, T. (2004). Occupational stress and coping among nurses. Journal of Health Management, 6, 115–127. doi:10.1177/097206340400600204
Potter, P., Deshields, T., Berger, J.A., Clarke, M., Olsen, S., & Chen, L. (2013). Evaluation of a compassion fatigue resiliency program for oncology nurses. Oncology Nursing Forum, 40, 180–187. doi:10.1188/13.ONF.180-187
Potter, P., Deshields, T., Divanbeigi, J., Berger, J., Cipriano, D., Norris, L., & Olsen, S. (2010). Compassion fatigue and burnout [Online exclusive]. Clinical Journal of Oncology Nursing, 14, E56–E62. doi:10.1188/10.CJON.E56-E62
Quattrin, R., Zanini, A., Nascig, E., Annunziata, M.A., Calligaris, L., & Brusaferro, S. (2006). Level of burnout among nurses working in oncology in an Italian region. Oncology Nursing Forum, 33, 815–820. doi:10.1188/06.ONF.815-820
Rodrigues, A.B., & Chaves, E.C. (2008). Stressing factors and coping strategies used by oncology nurses. Revista Latino-Americana de Enfermagem, 16, 24–28.
Sabo, B.M. (2008). Adverse psychosocial consequences: Compassion fatigue, burnout and vicarious traumatization: Are nurses who provide palliative and hematological cancer care vulnerable? Indian Journal of Palliative Care, 14, 23–29.
Traeger, L., Park, E.R., Sporn, N., Repper-DeLisi, J., Convery, M.S., Jacobo, M., & Pirl, W.F. (2013). Development and evaluation of targeted psychological skills training for oncology nurses in managing stressful patient and family encounters [Online exclusive]. Oncology Nursing Forum, 40, E327–E336.




