The Effect of Acceptance and Commitment Therapy–Based Psychoeducation on Body Image, Quality of Sexual Life, and Dyadic Adjustment of Women After Breast Cancer Surgery
Objectives: To determine the effect of acceptance and commitment therapy–based psychoeducation applied to women who have undergone breast cancer surgery on body image, quality of sexual life, and dyadic adjustment.
Sample & Setting: Women who have undergone breast cancer surgery were included. The research had a single-group quasi-experimental design with pre-/post-test measurements and 31 participants.
Methods & Variables: The research was carried out between February and July 2021. Data were collected using a personal information form, a body image perception scale, the Dyadic Adjustment Scale, and the Sexual Quality of Life–Female.
Results: The post-test mean scores of body image, quality of sexual life, and dyadic adjustment scales were significantly higher than pretest (p < 0.05).
Implications for Nursing: To improve the body image, quality of sexual life, and dyadic adjustment of women who have undergone breast cancer surgery, nurses are recommended to include psychoeducation based on acceptance and commitment therapy interventions in the nursing care process and to evaluate the effectiveness.
Jump to a section
Breast cancer is the most prevalent type of cancer globally (World Health Organization, 2022). In the United States, about 287,500 new cases of breast cancer were detected in 2022, resulting in the death of 43,550 women (National Breast Cancer Foundation, 2023). Similarly, cancer diseases are the second leading cause of death in Turkey, and breast cancer is the most prevalent type of cancer in women (Republic of Türkiye Ministry of Health, 2020). The methods used in the treatment of breast cancer are chemotherapy, radiation therapy, adjuvant therapy, hormone therapy, biologic agents, and surgical treatment (Göktaş, 2021). Studies show that women experience many problems after breast cancer surgery and difficulties particularly arising from psychosocial problems (Christophe et al., 2016; Rottmann et al., 2015). Psychotherapy interventions are frequently used to overcome the difficulties experienced with these psychosocial problems (LeRoy et al., 2018; Nikbakhsh et al., 2018).
Acceptance and commitment therapy (ACT) is a therapy model characterized as the third wave of cognitive behavioral therapies, proven to be effective on the psychological reflections of physical disorders such as cancer, as well as psychiatric disorders (Enoch & Nicholson, 2020; Fernández-Rodríguez et al., 2021; Mohabbat-Bahar et al., 2015). It has been reported that ACT can be an effective psychotherapeutic intervention for use in oncology; reduce various symptoms, such as psychological suffering, mood disorders, trauma, and physical pain; and increase quality of life and psychological flexibility (Fashler et al., 2018). For this reason, it is thought that ACT may also be effective on the psychosocial problems experienced by individuals during the breast cancer treatment process (Ahmadzadeh et al., 2019; Mahdavi et al., 2017; Mohabbat-Bahar et al., 2015). ACT supports individuals in displaying behaviors based on values that play a key role in their lives, by emphasizing willingness to accept feelings and thoughts related to difficult experiential life events (Gloster et al., 2020). The authors predicted that ACT-based psychoeducation would be effective on body image, quality of sexual life, and dyadic adjustment as known psychosocial problems.
Background
Body image refers to the perception, thoughts, feelings, and beliefs that individuals have about their own body. It includes how they perceive their appearance, size, shape, weight, and other physical attributes. Body image can have a significant impact on an individual’s mental and physical health, as well as their overall well-being (Cash, 2004; Secord & Jourard, 1953). It is reported that cancer-related body changes cause various problems in individuals; in particular, the change occurring in the breast affects body image and disrupts the perception of femininity, thereby negatively affecting the sexual functions and quality of sexual life in women (Kim & Jang, 2019).
Quality of sexual life refers to the subjective experience of satisfaction, pleasure, and fulfillment that individuals have in their sexual relationships. It encompasses various aspects of sexual functioning, such as desire, arousal, and intimacy. Factors that can influence the quality of sexual life include physical and psychological health, relationship dynamics, communication, and cultural and social norms (Blouet et al., 2019; Dosch et al., 2016). It is reported that breast cancer negatively affects a woman’s perception of gender (Kim & Jang, 2019). The relevant change in gender perception also causes changes in many role performances of women (Göktaş, 2021). For this reason, women also experience problems in their relationships with their partners (Brajkovic et al., 2021).
Dyadic adjustment refers to the quality of a romantic relationship between two individuals. It includes various aspects of the relationship, such as communication, intimacy, commitment, trust, and satisfaction. The level of dyadic adjustment can be influenced by many factors, including individual differences, life stressors, and relationship history. A high level of dyadic adjustment is generally associated with greater relationship satisfaction and overall well-being for both partners (Fişiloğlu & Demir, 2000; Girgin Büyükbayraktar & Kesici, 2020). A woman with a life-threatening disease has a condition that pushes her to a cancer-focused life and disrupts the dynamic of the spousal relationship (Brajkovic et al., 2021). Although many variables impair the physical sexual functions of women with breast cancer after surgery, any change in the woman’s body image and self-esteem or the reactions of her partner may have a significant effect on sexual function (Burwell et al., 2006; Chang et al., 2019; Marsh et al., 2020). Some women’s spouses may have difficulty looking at the incision area, which reinforces the woman’s fear that her body is deformed and disgusting (Zimmermann et al., 2010). In addition, women perceive the loss of all or part of the breast after the surgical intervention as a threat to their sexual identity and feel themselves sexually deficient or inadequate (Rayne et al., 2016). Finally, they experience fear and anxiety that their marital relations will be endangered and their emotional ties with their spouses will deteriorate, which is supported by studies (Brajkovic et al., 2021; Mahdavi et al., 2017).
Providing psychosocial support for women who have undergone breast cancer surgery is an essential nursing intervention. Therefore, ACT can be an effective method in psychosocial support of women with breast cancer (Han et al., 2019; Mani et al., 2019). ACT includes cognitive and behavioral processes and aims at psychological flexibility in individuals. Psychological flexibility contains the following six processes: present moment awareness, values, committed behaviors of a life consistent with determined values, acceptance, cognitive defusion, and a self as contextual (Gloster et al., 2020; Stockton et al., 2019). The ACT model involves willingness to have compulsory emotions and being aware of emotions for individuals (Çiçek & Tanhan, 2020; Vatan, 2016). In addition, the ACT model uses relational framework and functional context. Although the relational context determines what the person thinks, the functional context determines the psychological effect of the thought on the person. As with all other learning methods, learning by association never disappears once it occurs, but the effect of the associated stimuli on the person may fade (Enoch & Nicholson, 2020). With the breast cancer process, negative emotions and thoughts, particularly related to body image, can turn into a positive process with the effects of six basic areas of psychological flexibility in the current emotion/thought structure with the ACT approach. Acceptance of self-perception, flexible contact with the moment, and taking individual value-oriented actions can also provide partner harmony in the process and increase the quality of sexual life. For example, an individual with a value related to the belief of being a good partner can set goals and take action on the question of “How can I live the present moment more meaningfully with the current partner, willing to experience the emotions/thoughts brought about by this negative process?” (Christophe et al., 2016; Ghasemi & Jabalameli, 2020; Ghorbani et al., 2021; Han et al., 2019).
It was reported that women who had undergone breast cancer surgery were moderately satisfied with their body image, and the most frequently used coping strategy of these women was positive rational acceptance (Yamani Ardakani et al., 2020). In addition, a study was conducted with patients recovering from breast cancer to evaluate the acceptability and feasibility of adaptive cognitive behavioral therapy–based interventions in promoting positive body image. Improvements were identified at either post-test or one-month follow-up in nearly all body image measures, and the adapted intervention was acceptable and feasible for this group (Lewis-Smith et al., 2018). In other studies, ACT-based treatment was found to be effective in reducing marital conflict and improved the dyadic satisfaction of individuals with breast cancer (Ahmadzadeh et al., 2019; Mahdavi et al., 2017). Therefore, ACT-based approaches are expected to contribute to enhancing body image, quality of sexual life, and dyadic adjustment by providing psychological flexibility in women who have undergone breast cancer surgery. Although studies in the literature use ACT-based psychotherapy in women who have undergone breast cancer surgery (Blouet et al., 2019; Ghasemi & Jabalameli, 2020), no study has been found on the effects of ACT-based structured psychoeducation on body image, quality of sexual life, and dyadic adjustment.
Objectives
This study aims to determine the effect of ACT-based psychoeducation applied to patients undergoing breast cancer surgery on body image, quality of sexual life, and dyadic adjustment.
The following are the hypotheses of the research:
- H0: ACT-based psychoeducation applied to patients who have undergone breast surgery has no effect on body image, quality of sexual life, and dyadic adjustment.
- H1a: ACT-based psychoeducation applied to patients who have undergone breast surgery has a positive effect on body image.
- H1b: ACT-based psychoeducation applied to patients who have undergone breast surgery has a positive effect on quality of sexual life.
- H1c: ACT-based psychoeducation applied to patients who have undergone breast surgery has a positive effect on dyadic adjustment.
Methods
Design and Participants
The research has a single-group quasi-experimental design with pre-/post-test measurement. The research was carried out between February 10, 2021, and July 10, 2021, with women who had undergone surgery for breast cancer in a hospital in Samsun, Türkiye. The inclusion criteria for the participating women were as follows: having been diagnosed with stage I, II, or III breast cancer; having undergone surgery three months to five years ago; being married and living with a spouse; having a device and internet access to participate in psychoeducation sessions that would be held synchronously with Google Meet; having no diagnosis of medically determined neurologic or psychiatric disease; having undergone no reconstructive surgery after breast surgery (because of the impact on the independent variables); and having no disability that would prevent their participation in the study. The individuals who failed to participate in the pre-/post-tests and all the sessions were excluded from the study (see Figure 1).
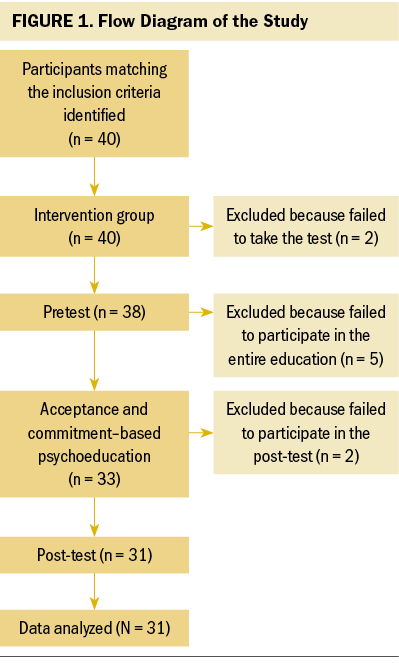
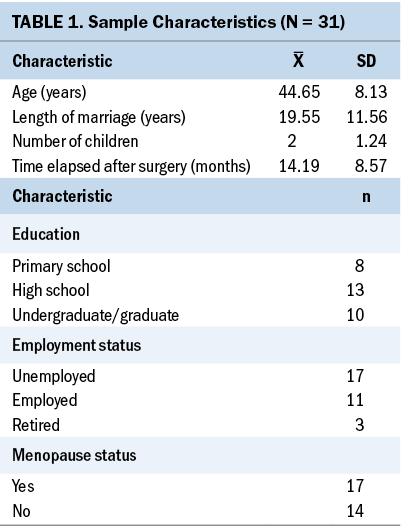
The sample size of the research was determined by analysis with G*Power, version 3.1. The sample size was calculated as 28 with 95% confidence interval, 5% margin of error, 0.72 effect size, and 95% power to represent the population (Ozdemir & Saritas, 2019). The study was started with 40 participants who met the inclusion criteria, and during the process, two participants who did not participate in the preliminary tests, five participants who did not participate in all psychoeducation training sessions, and two participants who did not participate in the final tests were excluded from the study. The sample was completed with 31 participants, reaching about 10% more than the sample size calculated (N = 28). The sociodemographic characteristics of the sample are shown in Table 1.
Data Collection
Personal information form: Prepared by the researchers after a literature review, the personal information form consists of seven questions including the introductory characteristics of individuals (e.g., age, education, length of marriage, time elapsed after breast cancer surgery) (Kim & Jang, 2019; Rottmann et al., 2015).
Body image perception scale: The Cronbach’s alpha coefficient of the body image perception scale (BIPS), which was developed by Secord and Jourard (1953) and whose validity and reliability studies were conducted by Hovardaoğlu (1993), is 0.95. The scale consists of 40 items, and scores range from 1 to 5 for each item. The total score of the scale ranges from 40 to 200. The cutoff score of the scale is 135. A high score indicates a high level of satisfaction, and scores below the cutoff score indicate low satisfaction with body image (Hovardaoğlu, 1993). In this study, the Cronbach’s alpha of the scale was determined to be 0.87.
Dyadic Adjustment Scale: The Dyadic Adjustment Scale (DAS), developed by Spanier (1976), was designed to measure the quality of the relationship as perceived by married or cohabiting couples. The Turkish validity and reliability study of the scale was done by Fişiloğlu and Demir (2000). The scale can be applied to each of the spouses separately—that is, as a single person. The Cronbach’s alpha of the scale is 0.9. The 32-item scale includes yes-or-no and Likert-type questions. The scale has the following four subscales: dyadic consensus, dyadic satisfaction, dyadic cohesion, and affective expression. The scale is measured over the total score and subscale scores. The distribution of the total score that can be obtained from the scale is 0–151. The scale has no cutoff score. The higher the total score, the better the individual’s relationship or dyadic adjustment. In the current study, measurement was made based on the total score of the scale. The Cronbach’s alpha value of the scale was determined to be 0.83.
Sexual Quality of Life–Female: The Sexual Quality of Life–Female (SQOL-F), developed by Symonds et al. (2005), was adapted into Turkish by Tuğut and Gölbaşı (2010). The Cronbach’s alpha of the 18-item scale is 0.83. The scale is a six-point Likert-type scale. In the current study, a scoring system between 1 and 6 was used as follows: 1 = strongly agree, 2 = moderately agree, 3 = slightly agree, 4 = slightly disagree, 5 = moderately disagree, and 6 = strongly disagree. The total score ranges from 18 to 108, with greater scores indicating higher quality of sexual life. In this study, the Cronbach’s alpha of the questionnaire was determined to be 0.86.
Intervention
ACT-based psychoeducation sessions, prepared in line with the opinions of authors who are experts in the field of psychiatric nursing, were held simultaneously with women who had undergone breast cancer surgery in six sessions via Google Meet (see Figure 2). To increase sharing and participation in psychoeducation sessions, women were divided into three groups, with a maximum of 11 people per session. Data collection tools created via Google Forms were sent to the women via email before the sessions began. After the pretests were applied, the ACT-based psychoeducation program was administered to the women online once a week for six weeks. One month after the last session, post-test measurements of the women were made via email.


In this program, group interaction was limited to individuals in the same group because all three groups were included in the intervention program at different times. However, the participants were encouraged to express themselves during the online program process, and it was stated by the participants that this situation positively affected the group interaction. In addition, individual assessments of the tasks given at the end of each online ACT session in the next session also contributed to group interaction. The online ACT sessions were planned considering the cultural characteristics of the people in the program. The metaphors used in the ACT, the examples in the sessions, and the fact that the online program was conducted as a group also showed that the problems were not experienced by only one person but that similar problems were experienced by many people with breast cancer. All these have contributed to increasing group interaction.
ACT-based psychoeducation sessions were conducted by researchers in the field of psychiatric nursing. Researchers had training on mindfulness-based psychological interventions (ACT, mindfulness-based stress reduction program). The researcher with an ACT certificate (36 hours of basic training; 60 hours of supervision) served as the first practitioner in all sessions.
Ethical Considerations
Before the study, ethical approval (2021/96; 29.01.2021) was obtained from Ondokuz Mayıs University Social and Human Sciences Research Ethics Committee and written permission was obtained from where the study was conducted (E-15374210-663.09-24121). Participants were informed about the study, and their written consent was obtained. Permission was obtained from the authors for the scales used in the study.
Data Analysis
The analysis of the research data was carried out with IBM SPSS Statistics, version 22.0, and G*Power, version 3.1. Power analysis was used for determining the number of samples (G*Power test). Skewness and kurtosis coefficients were used for determining the suitability of the data for the normal distribution. Cronbach’s alpha reliability coefficient was used to determine the total internal consistency coefficients of the scale. It was determined that the data showed normal distribution. One-way repeated measures analysis of variance (Wilks’s lambda test) was used to compare the pre- and post-test scores of the scales and to determine the effect level of the intervention. In addition, statistical analyses were carried out by an expert outside the research team to eliminate bias in the research.
Results
The average age of the individuals was 44.65 years (SD = 8.13), the average length of marriage was 19.55 years (SD = 11.56), the average number of children was 2 (SD = 1.24), and the average time elapsed after surgery was 14.19 months (SD = 8.57). In addition, 13 individuals were high school graduates, and 17 were unemployed and in the menopause period.
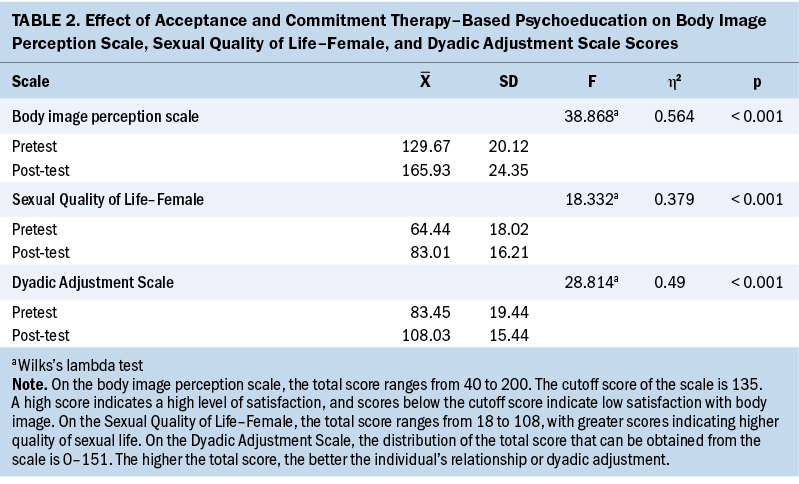
The effect of ACT-based psychoeducation applied to women who had undergone breast cancer surgery on BIPS, SQOL-F, and DAS scores was examined and is detailed in Table 2 and Figure 3.

The participants’ BIPS (Wilks’s lambda = F[1.3] = 38.868), SQOL-F (Wilks’s lambda = F[1.3] = 18.332), and DAS (Wilks’s lambda = F[1.3] = 28.814) post-test mean scores were found to be significantly higher than their pretest mean scores (p < 0.001). The women’s BIPS scores of the ACT-based psychoeducation program were 56% (eta squared = 0.564); their SQOL-F scores were 38% (eta squared = 0.379). It was determined that the ACT-based psychoeducation program increased DAS scores by 49% (eta squared = 0.49), creating a significant and wide effect.
Discussion
This study investigated the effectiveness of online ACT-based psychoeducation group training on psychosocial problems such as body image, quality of sexual life, and dyadic adjustment of people with breast cancer. Group intervention programs using ACT and methods based on the philosophy of mindfulness are effective in individuals accepting negative life experiences and emotions. The aim of this online group-based psychoeducation intervention is to provide psychological flexibility with the ACT model in women with breast cancer. Women with breast cancer who have gained psychological resilience can live voluntarily without trying to eliminate challenging emotions and experiences and can be freed from nonfunctional efforts.
All methods used in the oncologic treatment process create various changes on the body image of women with breast cancer. As a result, it negatively affects the body perceptions of women with breast cancer (Kołodziejczyk & Pawłowski, 2019). The first three months are important in terms of emotional disorders in women who have undergone adjuvant chemotherapy after breast cancer surgery because women with breast cancer have a high risk of deterioration in body image during this period (Słowik et al., 2017). These findings from the literature reveal the necessity of interventions aimed at gaining appropriate coping methods such as present-moment awareness and realistic acceptance in women undergoing surgery for breast cancer. In this study, it was determined that ACT-based psychoeducation applied to women after breast surgery was effective in increasing women’s body image satisfaction. When evaluated according to the BIPS cutoff score, it was determined that women’s satisfaction with body image was low before the ACT-based psychoeducation and the level of satisfaction increased significantly after the intervention. Similarly, in a study conducted with patients who underwent mastectomy, it was reported that ACT improved the body image of women in the experimental group (Ghasemi & Jabalameli, 2020).
There has been an increase in the number of studies assessing the effectiveness of ACT in improving symptoms in patients with breast cancer (Hadlandsmyth et al., 2019; Johns et al., 2020). However, there are still a limited number of studies assessing the effects of ACT-based interventions on the problems experienced by women in their relationship with their partners following breast cancer surgery (Ahmadzadeh et al., 2019; Mahdavi et al., 2017). This research shows that ACT-based psychoeducation applied to women after breast surgery is effective in increasing women’s dyadic satisfaction. In a randomized controlled study conducted with women diagnosed with breast cancer in Iran, it was found that ACT, which was applied to the experimental group for eight sessions, improved the dyadic satisfaction of the patients (Mahdavi et al., 2017). In another study conducted with 45 couples with breast cancer experience, ACT-based treatment was found to be effective in reducing marital conflict (Ahmadzadeh et al., 2019).
The quality of sexual life of women with breast cancer is affected after surgery. In this study, ACT-based psychoeducation applied to women after breast surgery was effective in improving the quality of women’s sexual life. The internet-based cognitive behavioral therapy intervention showed a significant improvement over time in overall sexual functioning, sexual desire, and sexual arousal for breast cancer survivors (Johns et al., 2020). Similarly, it was determined that group problem-solving therapy after mastectomy increased the effectiveness of women’s sexual function and satisfaction, and sexual health counseling was recommended (Bokaie et al., 2022). In studies in which it was reported that sexuality was among the important factors of quality of life, it was shown that the ACT intervention applied to people with breast cancer receiving chemotherapy was effective in improving quality of life in patients (Han et al., 2019; Hummel et al., 2017). Similarly, in an experimental study conducted with women diagnosed with breast cancer, it was found that ACT applied to the individuals in the experimental group increased the quality of life of the patients, and it was a new approach to improve the psychological state of patients with breast cancer (Mani et al., 2019).
The ACT-based psychoeducation was applied in the research in line with the principles of ACT. The use of this model was intended to prevent negative thinking from being accepted as a part of life and avoiding unpleasant experiences, rather than changing them (Fernández-Rodríguez et al., 2021). There was emphasis on mindfulness for improvement in psychological flexibility. All these methods enabled the participants to accept the positive as well as negative aspects of cancer. It can be inferred that the improvement in the patients’ body image, dyadic adjustment, and quality of sexual life is related to the adaptation of the ACT-based psychoeducation program applied to the group in line with the ACT principles.
ACT may be an effective model to promote empowerment of women in coping with breast cancer, and it can reduce psychological effects of the durations of problems.
Limitations
The most important limitation of the study was that it was conducted with 31 women. Another important limitation of the study is that it was conducted in a single center. In addition, this research was carried out with a quasi-experimental design with a single group. The fact that it was not carried out with a randomized controlled trial design is also a limitation.
Apart from all these limitations, difficulties were experienced at various times because of the disconnection of the internet during the implementation phase (sessions) of the study, which may negatively affect the willingness of the participants to participate in the sessions. However, no feedback on this situation was given by the participants. For this reason, the current flow process was adversely affected, albeit partially, by the disconnection during the implementation of the program.
Implications for Nursing
Cancer-related body changes cause various problems in individuals, and in particular, the change occurring in the breast affects body image. Providing psychosocial support for women who have undergone breast cancer surgery is an essential nursing intervention in an attempt to cope with the problems experienced in the postoperative period. ACT interventions applied to people with breast cancer warrant further study so nurses can provide effective psychosocial care for patients undergoing breast cancer surgery by improving their knowledge and skills on ACT-based approaches. It is important for clinical nurses working with women who have undergone breast cancer surgery to integrate psychosocial interventions in their nursing care. To do this, it is necessary for nurses to participate in psychosocial skill development training programs such as mindfulness, acceptance, compassion, self-compassion, and cognitive emotion regulation, in terms of quality of care. The ACT-based psychoeducation program that the authors applied to women who had undergone breast cancer surgery in the current study can be used as an example for nurses who have gained knowledge and skills about mindfulness-based interventions. Based on the topics included in the sessions of the program applied in this research, the techniques used can be diversified in line with individual and cultural variables. It can be used for many technical purposes, such as meditation and imagination practices, metaphors, pictures, and writing exercises.

Conclusion
The findings of this study reveal the positive effects of ACT-based psychoeducation on improving body image, sexual quality of life, and dyadic adjustment of women undergoing breast cancer surgery and inform nurses about the implementation of this intervention. Based on this research, ACT-based psychoeducation applied to women after breast cancer surgery increases the body image satisfaction level of about one in two women, the quality of sexual life of about one in three women, and the dyadic adjustment of about one in two women. Nurses can provide effective psychosocial care for individuals undergoing breast cancer surgery by improving their knowledge and skills on ACT-based approaches. When doing so, nurses can help patients to get to know themselves better, realize their situation, and improve their body image, quality of sexual life, and dyadic adjustment. The findings are expected to provide valuable information to nurses doing research on similar topics.
About the Authors
Ercan Tunç, PhD, is a research assistant, and Oya Sevcan Orak, PhD, is an associate professor, both in the Department of Psychiatric Nursing; and Özge İşeri, PhD, is an assistant professor in the Department of Surgical Diseases Nursing, all in the Faculty of Health Sciences at Ondokuz Mayıs University in Turkey. Tunç and Orak completed the data collection. All authors contributed to the conceptualization and design, provided statistical support and the analysis, and contributed to the manuscript preparation. Orak can be reached at oysev@hotmail.com, with copy to ONFEditor@ons.org. (Submitted August 2022. Accepted April 21, 2023.)
References
Ahmadzadeh, L., Vaezi, M., Sodagar, S.H., Bahrami Hidaji, M., & Golmohammad Nazhad Bahrami, G.H. (2019). The effect of acceptance and commitment therapy adopted for couples compared with integrative couple therapy on marital conflicts of couples with breast cancer. Iranian Quarterly Journal of Breast Disease, 12(3), 47–59. https://pdfs.semanticscholar.org/3fa5/e356d30c7c8fb93eac4134c2283a0def5…
Blouet, A., Zinger, M., Capitain, O., Landry, S., Bourgeois, H., Seegers, V.T., & Pointreau, Y. (2019). Sexual quality of life evaluation after treatment among women with breast cancer under 35 years old. Supportive Care in Cancer, 27(3), 879–885. https://doi.org/10.1007/s00520-018-4374-z
Bokaie, M., Firouzabadi, O., & Joulaee, A. (2022). The effectiveness of group problem-solving therapy on women’s sexual function and satisfaction after mastectomy surgery. BMC Women’s Health, 22(50), 1–7. https://doi.org/10.1186/s12905-022-01628-x
Brajkovic, L., Sladic, P., & Kopilaš, V. (2021). Sexual quality of life in women with breast cancer. Health Psychology Research, 9(1), 24512. https://doi.org/10.52965/001c.24512
Burwell, S.R., Case, L.D., Kaelin, C., & Avis, N.E. (2006). Sexual problems in younger women after breast cancer surgery. Journal of Clinical Oncology, 24(18), 2815–2821. https://doi.org/10.1200/JCO.2005.04.2499
Cash, T.F. (2004). Body image: Past, present, and future. Body Image, 1(1), 1–5. https://doi.org/10.1016/S1740-1445(03)00011-1
Chang, Y.-C., Chang, S.-R., & Chiu, S.-C. (2019). Sexual problems of patients with breast cancer after treatment: A systematic review. Cancer Nursing, 42(5), 418–425. https://doi.org/10.1097/NCC.0000000000000592
Christophe, V., Duprez, C., Congard, A., Fournier, E., Lesur, A., Antoine, P., & Vanlemmens, L. (2016). Evaluate the subjective experience of the disease and its treatment in the partners of young women with non-metastatic breast cancer. European Journal of Cancer Care, 25(5), 734–743. https://doi.org/10.1111/ecc.12327
Çiçek, İ., & Tanhan, A. (2020). Terapide paradoksal müdahaleler. Adıyaman Üniversitesi Sosyal Bilimler Enstitüsü Dergisi, 13(36), 383–411. https://doi.org/10.14520/adyusbd.684096
Dosch, A., Rochat, L., Ghisletta, P., Favez, N., & Van der Linden, M. (2016). Psychological factors involved in sexual desire, sexual activity, and sexual satisfaction: A multi-factorial perspective. Archives of Sexual Behavior, 45(8), 2029–2045. https://doi.org/10.1007/s10508-014-0467-z
Enoch, M.R., & Nicholson, S.L. (2020). Acceptance and commitment therapy and relational frame theory in the field of applied behavior analysis: The acceptability and perspective of the practicing BCBA. Behavior Analysis in Practice, 13(3), 609–617. https://doi.org/10.1007/s40617-020-00416-z
Fashler, S.R., Weinrib, A.Z., Azam, M.A., & Katz, J. (2018). The use of acceptance and commitment therapy in oncology settings: A narrative review. Psychological Reports, 121(2), 229–252. https://doi.org/10.1177/0033294117726061
Fernández-Rodríguez, C., González-Fernández, S., Coto-Lesmes, R., & Pedrosa, I. (2021). Behavioral activation and acceptance and commitment therapy in the treatment of anxiety and depression in cancer survivors: A randomized clinical trial. Behavior Modification, 45(5), 822–859. https://doi.org/10.1177/0145445520916441
Fişiloğlu, H., & Demir, A. (2000). Applicability of the dyadic adjustment scale for measurement of marital quality with Turkish couples. European Journal of Psychological Assessment, 16(3), 214–218. https://psycnet.apa.org/doi/10.1027/1015-5759.16.3.214
Ghasemi, L., & Jabalameli, S. (2020). Effectiveness of acceptance and commitment therapy on body image in women with breast cancer after mastectomy surgery. Journal of Health System Research, 15(4), 255–261. https://doi.org/10.32592/hsr.2020.15.4.101
Ghorbani, V., Zanjani, Z., Omidi, A., & Sarvizadeh, M. (2021). Efficacy of acceptance and commitment therapy (ACT) on depression, pain acceptance, and psychological flexibility in married women with breast cancer: A pre- and post-test clinical trial. Trends in Psychiatry and Psychotherapy, 43(2), 126–133. https://doi.org/10.47626/2237-6089-2020-0022
Girgin Büyükbayraktar, Ç., & Kesici, Ş. (2020). Commitment of married couples in marriage and dyadic adjustment prediction of commitment styles. Research on Education and Psychology, 4(2), 133–152. https://dergipark.org.tr/en/download/article-file/877406
Gloster, A.T., Walder, N., Levin, M.E., Twohig, M.P., & Karekla, M. (2020). The empirical status of acceptance and commitment therapy: A review of meta-analyses. Journal of Contextual Behavioral Science, 18, 181–192. https://doi.org/10.1016/j.jcbs.2020.09.009
Göktaş, S. (2021). Meme cerrahisinde bakım. In M. Karadağ & H. Bulut (Eds.), Kavram haritası ve akış şemalı cerrahi hemşireliği (pp. 933–987). Vize Publishing.
Hadlandsmyth, K., Dindo, L.N., Wajid, R., Sugg, S.L., Zimmerman, M.B., & Rakel, B.A. (2019). A single-session acceptance and commitment therapy intervention among women undergoing surgery for breast cancer: A randomized pilot trial to reduce persistent postsurgical pain. Psycho-Oncology, 28(11), 2210–2217. https://doi.org/10.1002/pon.5209
Han, J., Liu, J.-E., Su, Y.-L., & Qiu, H. (2019). Effect of a group-based acceptance and commitment therapy (ACT) intervention on illness cognition in breast cancer patients. Journal of Contextual Behavioral Science, 14, 73–81. https://doi.org/10.1016/j.jcbs.2019.09.003
Hovardaoğlu, S. (1993). Body image scale. 3P, 1(1), 26.
Hummel, S.B., van Lankveld, J.J.D.M., Oldenburg, H.S.A., Hahn, D.E.E., Kieffer, J.M., Gerritsma, M.A., . . . Aaronson, N.K. (2017). Efficacy of internet-based cognitive behavioral therapy in improving sexual functioning of breast cancer survivors: Results of a randomized controlled trial. Journal of Clinical Oncology, 35(12), 1328–1340. https://doi.org/10.1200/jco.2016.69.6021
Johns, S.A., Stutz, P.V., Talib, T.L., Cohee, A.A., Beck-Coon, K.A., Brown, L.F., . . . Giesler, R.B. (2020). Acceptance and commitment therapy for breast cancer survivors with fear of cancer recurrence: A 3-arm pilot randomized controlled trial. Cancer, 126(1), 211–218. https://doi.org/10.1002/cncr.32518
Kim, J., & Jang, M. (2019). Stress, social support, and sexual adjustment in married female patients with breast cancer in Korea. Asia-Pacific Journal of Oncology Nursing, 7(1), 28–35. https://doi.org/10.4103/apjon.apjon_31_19
Kołodziejczyk, A., & Pawłowski, T. (2019). Negative body image in breast cancer patients. Advances in Clinical and Experimental Medicine, 28(8), 1137–1142. https://doi.org/10.17219/acem/103626
LeRoy, A.S., Shields, A., Chen, M.A., Brown, R.L., & Fagundes, C.P. (2018). Improving breast cancer survivors’ psychological outcomes and quality of life: Alternatives to traditional psychotherapy. Current Breast Cancer Reports, 10(1), 28–34. https://doi.org/10.1007/s12609-018-0266-y
Lewis-Smith, H., Diedrichs, P.C., & Harcourt, D. (2018). A pilot study of a body image intervention for breast cancer survivors. Body Image, 27, 21–31. https://doi.org/10.1016/j.bodyim.2018.08.006
Mahdavi, A., Aghaei, M., Aminnasab, V., Tavakoli, Z., Besharat, M., & Abedin, M. (2017). The effectiveness of acceptance-commitment therapy (ACT) on perceived stress, symptoms of depression, and marital satisfaction in women with breast cancer. Archives of Breast Cancer, 4(1), 16–23. https://doi.org/10.19187/abc.20174116-23
Mani, A., Mehdipour, Z., Ahmadzadeh, L., Tahmasebi, S., Khabir, L., & Mosalaei, A. (2019). The effectiveness of group acceptance and commitment psychotherapy on psychological well-being of breast cancer patients in Shiraz, Iran. Middle East Journal of Cancer, 10(3), 231–238. https://doi.org/10.30476/mejc.2019.45316
Marsh, S., Borges, V.F., Coons, H.L., & Afghahi, A. (2020). Sexual health after a breast cancer diagnosis in young women: Clinical implications for patients and providers. Breast Cancer Research and Treatment, 184(3), 655–663. https://doi.org/10.1007/s10549-020-05880-3
Mohabbat-Bahar, S., Maleki-Rizi, F., Akbari, M.E., & Moradi-Joo, M. (2015). Effectiveness of group training based on acceptance and commitment therapy on anxiety and depression of women with breast cancer. Iranian Journal of Cancer Prevention, 8(2), 71–76. https://pubmed.ncbi.nlm.nih.gov/25960844
National Breast Cancer Foundation. (2023). Breast cancer facts and stats. https://www.nationalbreastcancer.org/breast-cancer-facts
Nikbakhsh, N., Moudi, S., Alvarzandi, S., Niazifar, M., Farnoush, N., Bijani, A., & Moudi, M. (2018). Citalopram and group psychotherapy in breast cancer patients: A randomized clinical trial. Medical Journal of the Islam Republic of Iran, 32, 68. https://doi.org/10.14196/mjiri.32.68
Ozdemir, A., & Saritas, S. (2019). Effect of yoga nidra on the self-esteem and body image of burn patients. Complementary Therapies in Clinical Practice, 35, 86–91. https://doi.org/10.1016/j.ctcp.2019.02.002
Rayne, S., Schnippel, K., Firnhaber, C., Wright, K., Kruger, D., & Benn, C.-A. (2016). Fear of treatments surpasses demographic and socioeconomic factors in affecting patients with breast cancer in urban South Africa. Journal of Global Oncology, 3(2), 125–134. https://doi.org/10.1200/JGO.2015.002691
Republic of Türkiye Ministry of Health. (2020). Health statistics yearbook 2020. General Directorate of Health Information Systems. https://dosyasb.saglik.gov.tr/Eklenti/43400,siy2020-eng-26052022pdf.pdf…
Rottmann, N., Hansen, D.G., Larsen, P.V., Nicolaisen, A., Flyger, H., Johansen, C., & Hagedoorn, M. (2015). Dyadic coping within couples dealing with breast cancer: A longitudinal, population-based study. Health Psychology, 34(5), 486–495. https://doi.org/10.1037/hea0000218
Secord, P.F., & Jourard, S.M. (1953). The appraisal of body-cathexis: Body-cathexis and the self. Journal of Consulting Psychology, 17(5), 343–347. https://doi.org/10.1037/h0060689
Słowik, A.J., Jabłoński, M.J., Michałowska-Kaczmarczyk, A.M., & Jach, R. (2017). Evaluation of quality of life in women with breast cancer, with particular emphasis on sexual satisfaction, future perspectives and body image, depending on the method of surgery. Psychiatria Polska, 51(5), 871–888. https://doi.org/10.12740/PP/OnlineFirst/63787
Spanier, G.B. (1976). Measuring dyadic adjustment: New scales for assessing the quality of marriage and similar dyads. Journal of Marriage and Family, 38(1), 15–28. https://doi.org/10.2307/350547
Stockton, D., Kellett, S., Berrios, R., Sirois, F., Wilkinson, N., & Miles, G. (2019). Identifying the underlying mechanisms of change during acceptance and commitment therapy (ACT): A systematic review of contemporary mediation studies. Behavioural and Cognitive Psychotherapy, 47(3), 332–362. https://doi.org/10.1017/S1352465818000553
Symonds, T., Boolell, M., & Quirk, F. (2005). Development of a questionnaire on sexual quality of life in women. Journal of Sex and Marital Therapy, 31(5), 385–397. https://doi.org/10.1080/00926230591006502
Tuğut, N., & Gölbaşı, Z. (2010). A validity and reliability study of Turkish version of the sexual quality of life questionnaire-female. Cumhuriyet Medical Journal, 32(2), 172–180. https://doi.org/10.1136/bmj.2.918.172
Vatan, S. (2016). Third wave of cognitive behavioral therapies. Current Approaches in Psychiatry, 8(3), 190–203. https://doi.org/10.18863/pgy.238183
World Health Organization. (2022). Cancer. https://www.who.int/news-room/fact-sheets/detail/cancer
Yamani Ardakani, B., Tirgari, B., & Roudi Rashtabadi, O. (2020). Body image and its relationship with coping strategies: The views of Iranian breast cancer women following surgery. European Journal of Cancer Care, 29(1), e13191. https://doi.org/10.1111/ecc.13191
Zimmermann, T., Scott, J.L., & Heinrichs, N. (2010). Individual and dyadic predictors of body image in women with breast cancer. Psycho-Oncology, 19(10), 1061–1068. https://doi.org/10.1002/pon.1660



