Pain and Spirituality Outcomes Among Women With Advanced Breast Cancer Participating in a Foot Reflexology Trial
Objectives: To examine pain and spirituality, demographic and clinical factors associated with pain and spirituality, the contribution of spirituality to experiences of pain over time, and how pain and spirituality relate to engagement with a caregiver-delivered intervention.
Sample & Setting: Women with advanced breast cancer (N = 256) enrolled in a home-based randomized controlled trial of foot reflexology.
Methods & Variables: Secondary analyses were conducted with baseline and postintervention data. Stepwise model building, linear mixed-effects modeling, and negative binomial regression were used.
Results: Participants who were younger, not married or partnered, not employed, or receiving hormonal therapy had increased odds of higher pain levels. Those who were older, non-White, or Christian had increased odds of higher spirituality. Spirituality’s contribution to pain was not significant over time.
Implications for Nursing: Women in this sample experienced moderate pain, on average, at baseline. Women with specific demographic and clinical characteristics may require additional support with pain management and spiritual care.
Jump to a section
Pain is a distressing experience with interacting sensory, cognitive, and emotional components, which may be associated with actual or perceived tissue damage (Bushnell et al., 2013; International Association for the Study of Pain, 1979; Wang et al., 2016; Williams & Craig, 2016). As many as 83% of women with advanced breast cancer report pain (Puetzler et al., 2014), indicating that novel approaches to managing pain in this population are needed. Pain can be the result of cancer, treatment, or comorbidities (Posternak et al., 2016), and it can adversely affect an individual’s quality of life (QOL) (Rodriguez et al., 2019). Spirituality may positively alter the experience of pain in women with advanced breast cancer, but this is one area that has not yet been adequately investigated (Flanigan et al., 2019; Visser et al., 2018). The overarching purpose of this study is to examine the contribution of spirituality to experiences of pain over time in these women.
Conceptually, this study is grounded in an adaptation of Reed’s (2015) theory of self-transcendence, a theory that has been applied in various samples of individuals with breast cancer (Matthews & Cook, 2009; Thomas et al., 2010). In the theory of self-transcendence, vulnerability (awareness of mortality) serves as a resource to enhance self-transcendence (expand self-boundaries in various ways), and self-transcendence helps to facilitate well-being (subjective feeling of health or wholeness). Personal and contextual factors may influence other components of the model (Reed, 2015). Modified and applied to this work, spirituality is an expression of self-transcendence, pain level is the outcome indicating one aspect of well-being (where lower pain serves as an indicator of higher well-being), and demographic and clinical factors may contribute to pain and spirituality.
Literature Review
Managing pain associated with cancer can be costly (Meads et al., 2019). Pain can also result in significant suffering (Can et al., 2019), so understanding spirituality’s contribution to the experience of pain may open avenues to innovative interventions. Spirituality is a dynamic process whereby humans experience connection with self, others, nature or a higher power, and a sense of meaning (Steinhauser et al., 2017; Sun Ko et al., 2017; Weathers et al., 2016); it may serve as a resource when facing cancer and its associated symptoms (Flanigan et al., 2019; Visser et al., 2018). Women with advanced breast cancer have indicated that spirituality serves as a resource when facing their disease (Gaston-Johansson et al., 2013). Spirituality can positively alter the disease experience; therefore, it may also serve as a resource for altering pain experiences (Flanigan et al., 2019; Visser et al., 2018). Spirituality can be significant throughout the lifespan but often becomes particularly important when faced with a life-threatening disease, such as advanced cancer (Balducci, 2019).
Enhancing spirituality is hypothesized to alter negative thoughts and emotions associated with pain, modulating the cognitive and emotional components and transforming the painful experience. Because pain is constructed of interacting sensory, cognitive, and emotional components, altering any of these carries the potential to modulate the pain experience (Zeidan & Vargo, 2016). Previous studies have built support for this hypothesis, indicating that thoughts and emotions play a profound role in how pain is experienced (Bushnell et al., 2013). Evidence suggests that spirituality offers a route to positive thoughts and emotions, such as a sense of safety and security, when facing difficult circumstances (Renz et al., 2018; Yeager et al., 2016). Multiple studies have reported significant relationships between pain and spirituality in varying samples of individuals with cancer (Bai et al., 2018; Delgado-Guay et al., 2016; Wang & Lin, 2016). This work builds on these findings and extends the inquiry to a population of women with advanced breast cancer enrolled in a complementary and integrative health (CIH) intervention trial.
CIH interventions focus on caring for the mind, body, and spirit holistically, recognizing that these are interrelated (National Cancer Institute, 2019). Reflexology is the CIH intervention included in this study. Reflexology entails applying firm pressure to specific points on the feet or hands, corresponding to different parts of the body (National Cancer Institute, 2019; Reflexology Association of America, 2018). The underlying mechanisms are not yet well understood; it is postulated that stimulating these reflexes alters various biologic and energetic pathways, causing physiologic changes, which positively alter symptoms (Wyatt et al., 2017). CIH interventions, such as reflexology, may also elicit the body’s innate healing abilities (McGrady & Moss, 2018). A longitudinal randomized controlled trial (RCT) of foot reflexology found significant decreases in pain over time among women with advanced breast cancer receiving the standardized reflexology intervention, compared to women in the control group (Wyatt et al., 2017). Despite energetic and spiritual underpinnings of the reflexology intervention, the level of self-reported spirituality has not been found to significantly change over time among women receiving reflexology (versus controls) (Flanigan & Cui, 2019).
Spirituality may also alter the experience of pain through a lesser-studied behavioral route, potentially enhancing the uptake of pain management interventions, thereby indirectly influencing pain. The current study examines this hypothesis within the context of a CIH-based reflexology intervention. Research suggests that those with higher self-reported spirituality report using more self-management interventions (Harvey, 2008; Yeager et al., 2016; Zarei et al., 2015). In addition, higher self-reported spirituality may be associated with greater openness toward CIH interventions (Smith et al., 2008). Because CIH interventions have inherent spiritual underpinnings (McGrady & Moss, 2018; National Cancer Institute, 2019), women with higher self-reported spirituality may be more likely to engage than those with lower self-reported spirituality. Therefore, it is hypothesized that spirituality may directly contribute to pain experiences through alterations in thoughts and emotions, and indirectly alter pain by enhancing the uptake of a CIH-based pain management intervention (reflexology).
Because pain and spirituality are highly individual experiences, they may be influenced by demographic and clinical factors. Preliminary work examining demographic and clinical factors in relation to pain and spirituality within varying populations has yielded mixed results (Mystakidou et al., 2008; Posternak et al., 2016). Although various demographic and clinical factors may be important predictors of unmanaged pain or issues with spirituality, a gap exists in understanding some potentially important demographic and clinical factors in women with advanced breast cancer. Therefore, this work examines pain and spirituality in a sample of women with advanced breast cancer who are enrolled in a CIH intervention trial, while considering potentially significant demographic and clinical factors. The study objectives were as follows:
• Determine the level of pain and the level of spirituality at baseline, prior to engaging in reflexology.
• Examine which demographic and clinical factors were associated with pain and with spirituality at baseline.
• Explore the impact of spirituality on pain over time (baseline through week 11), in the reflexology group versus the control group, when controlling for demographic and clinical factors.
• Distinguish how pain level and spirituality may affect engagement in the CIH-based reflexology intervention over time (baseline, week 5, and week 11), when controlling for demographic and clinical factors.
Methods
Sample and Setting
A secondary analysis was conducted from “Home-Based Symptom Management via Reflexology for Advanced Breast Cancer Patients” (5R01CA157459-05) (Wyatt, 2011–2018). This longitudinal RCT examined the effects of caregiver-delivered foot reflexology on symptoms and QOL (Wyatt et al., 2017). Participants were recruited from nine community-based oncology clinics and two comprehensive cancer centers in the Midwest. Inclusion criteria were as follows: being aged 21 years or older, being diagnosed with advanced breast cancer, being able to perform basic activities of daily living, having had received a first chemotherapy infusion, being able to speak and understand English, having access to a telephone, being able to hear normal conversation, being cognitively oriented, and having a friend or family member who is willing to participate. Exclusion criteria were as follows: being diagnosed with a major mental illness, residing in a nursing home, being bedridden, receiving regular reflexology, or having diagnoses or symptoms of deep vein thrombosis or painful foot neuropathy. This secondary analysis included data from 256 women (n = 128 reflexology, n = 128 control at baseline). See Figure 1 for an overview of study enrollment. 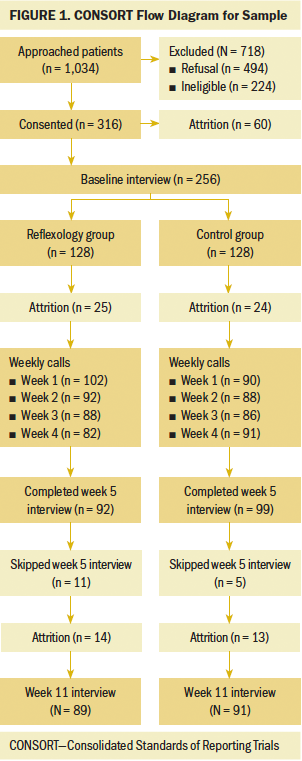
Variables
Approval from institutional review boards was obtained before beginning research. Nurse recruiters provided information to eligible women, inviting them to participate with a friend or family caregiver (comprising a dyad). After the baseline interview, participants were randomized using minimization procedure to one of the following two groups:
• Reflexology: receiving four weeks of home-based, lay caregiver–delivered foot reflexology (following a 30-minute foot reflexology protocol), and symptom assessment calls
• Attention control: receiving four weekly symptom assessment calls only
At the start of study participation, lay caregivers whose dyads were randomized to the reflexology group were trained in the standardized foot reflexology protocol at home by a certified reflexologist. Dyads were encouraged to complete at least one home-based foot reflexology session together per week throughout the study period.
Each woman participated in the study with her friend or family caregiver for 11 weeks. Data were collected via telephone by trained interviewers at baseline, week 5, and week 11, and during weekly symptom assessment calls (weeks 2–5). Weekly calls assessed the severity and interference of common cancer symptoms (including pain), as well as the number of reflexology sessions completed since the last call. Weeks 2–5 were considered the active intervention period, during which weekly calls reminded women to engage in reflexology. Weeks 6–11 were considered the maintenance period, to examine intervention sustainability without weekly calls. A review of the medical record was also completed. The parent study collected additional data, but only data relevant to this secondary analysis are reported here.
Measures
Pain: Pain was assessed using the PROMIS® (Patient-Reported Outcomes Measurement Information System)-29 Profile v1.0 pain intensity item (“In the past seven days, how would you rate your pain on average?”) at baseline and weeks 5 and 11 (HealthMeasures, 2018). Pain was rated from 0 (no pain) to 10 (worst imaginable pain). Extensive testing of reliability and validity has been conducted on the PROMIS-29 Profile v1.0, yielding strong evidence of validity and high internal consistency (Cronbach’s alpha = 0.92–0.96) in a large study of individuals with cancer (Jensen et al., 2015). In this work, the following cut points were adopted: mild = 1, moderate = 2–4, and severe = 5–10. These were developed to indicate clinically meaningful changes in pain among a large sample of individuals with cancer (Given et al., 2008).
Spirituality: Spirituality was assessed using the Long-Term QOL (LTQL)–spiritual/philosophical subscale. The LTQL was developed based on four dimensions of QOL (Ferrell et al., 1991) and focus groups (Wyatt et al., 1996). The LTQL is comprised of four subscales: somatic, spiritual/philosophical, health habits, and social/emotional (Wyatt & Friedman, 1996). The spiritual/philosophical subscale contains 11 items reflecting increased insight and appreciation (connection with self, others, higher power, nature, and meaning) (Wyatt et al., 1996; Wyatt & Friedman, 1996). Items are measured on a five-point scale, with 0 indicating low self-reported spirituality and 4 indicating high self-reported spirituality. Significant correlation with Cancer Rehabilitation Evaluation System, a cancer-specific QOL measure (Ganz et al., 1992), established evidence of validity of the LTQL (Wyatt et al., 1996). A separate study with this same sample of women showed high reliability on the LTQL spiritual/philosophical subscale (a = 0.8) (Kamp et al., 2019).
Demographic and clinical factors: Demographic and clinical factors were assessed at baseline using a standardized demographics form and a chart review form, both developed for the parent study. The demographics form elicited information on education, racial/ethnic background, religious preference, marital status, menopausal status, and employment status. Items were assessed via self-report using multiple-choice format. The chart review collected information on participant age, disease stage, metastasis, recurrence, and treatment type. Data were abstracted from medical records by a trained study team member.
Number of reflexology sessions: Number of 30-minute foot reflexology sessions was assessed during weekly calls in weeks 2–5 and during the week 11 interview (assessing sessions completed in weeks 6–11). Participants self-reported the number of sessions completed with their lay caregiver, which was transcribed onto a standardized form. The number of sessions was pooled for weeks 2–5 and 6–11, reflecting the active intervention versus maintenance period.
Analyses
IBM SPSS Statistics, version 25.0, and R, version 3.6.1, were used for analysis. Each analysis was conducted using available case analysis, including data from all cases where required variables were present in the data set. Descriptive statistics were initially examined to describe the sample.
Aim 1: To examine baseline levels of pain and spirituality in this sample of women, means (with standard deviation and variance) were calculated using the entire sample at baseline.
Aim 2: Two separate models were constructed (ordinal regression for pain, truncated regression for spirituality), using stepwise model building procedures. These tests were based on the hypothesis that multiple different demographic factors (age, education, racial/ethnic background, religious preference, marital status, employment status) and clinical factors (disease stage, metastasis, recurrence, treatment type, menopausal status) may be associated with spirituality or pain.
Aim 3: A linear mixed-effects model was used, accounting for within-person correlation between time points. Spirituality served as the independent variable and pain as a dependent variable, with selected demographic and clinical factors as covariates. The intervention group (reflexology versus control) was included as a moderator, testing the interaction between reflexology and time on pain. A three-way interaction among group, time, and spirituality was also tested. It was hypothesized that higher spirituality would contribute to a lower pain level, and that the effect would be stronger in the reflexology group.
Aim 4: Negative binomial regression was conducted, with pain group (mild, moderate, or severe) as an additional variable. Selected demographic and clinical factors were added as covariates. A two-way interaction between pain and spirituality was tested. Two regressions were conducted, one examining baseline pain and spirituality in relation to number of sessions completed in weeks 2–5, and one examining week 5 pain and spirituality in relation to number of sessions completed in weeks 6–11. These tests were based on the hypothesis that higher spirituality would be a significant predictor of greater number of reflexology sessions performed at each point, regardless of pain level.
Results
Descriptive statistics for this sample are displayed in Table 1. Participants had a mean age of 55.7 years and predominantly were White, were married, and had metastatic breast cancer, and they were most often receiving chemotherapy or targeted therapy. 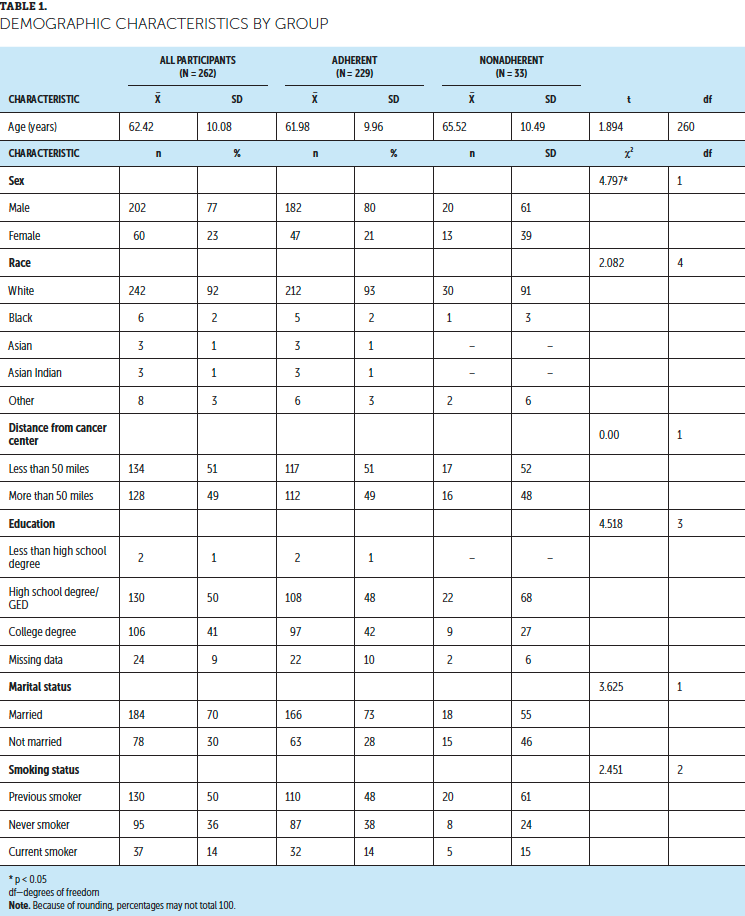
Aim 1: For the reflexology group, mean pain was 3.57 (SD = 2.59) and mean spirituality was 3.18 (SD = 0.7). For the control group, mean pain was 3.63 (SD = 2.83) and mean spirituality was 3.22 (SD = 0.56).
Aim 2: Ordinal and truncated regressions revealed that some demographic and clinical factors were associated with pain and spirituality (see Table 2). For pain, the demographic and clinical factors significantly associated with pain level were age (p < 0.03), marital status (p < 0.01), employment status (p < 0.00), and treatment type (p < 0.02). Results revealed that participants who were younger, not married or living with a partner, not employed or responded “other” to their employment status, or receiving hormonal therapy had a slight increase in ordered log odds of having a higher level of pain. For spirituality, the demographic and clinical factors significantly associated with spirituality level were age (p < 0.00), race (p < 0.05), and religious preference (p < 0.00). Results revealed that participants who were older, not White, or Christian had increased odds of having a higher level of spirituality. 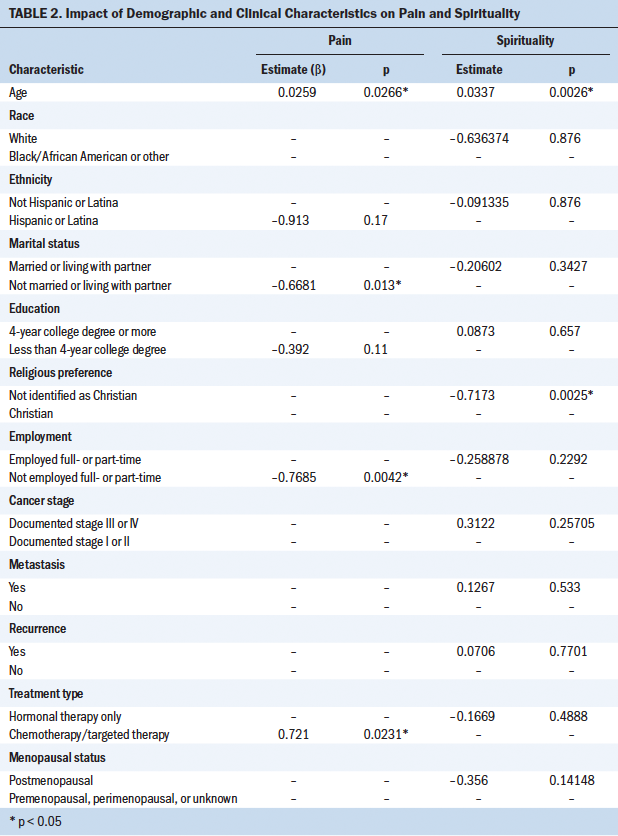
Aim 3: Self-reported spirituality was not significantly associated with level of pain in this sample of women (see Table 3). The three-way interaction among study group, time, and spirituality was not found to be significant and, thereby, was not included in the table. The two-way interaction between study group and time was significant (p < 0.04), indicating a significant change in pain over time across the groups. However, the intervention’s effect on pain cannot be discerned from these results (see Wyatt et al. [2017] for a detailed report of intervention effects). Finally, age, marital status, employment status, and treatment type were found to be significantly associated with pain, underscoring the results of aim 2. 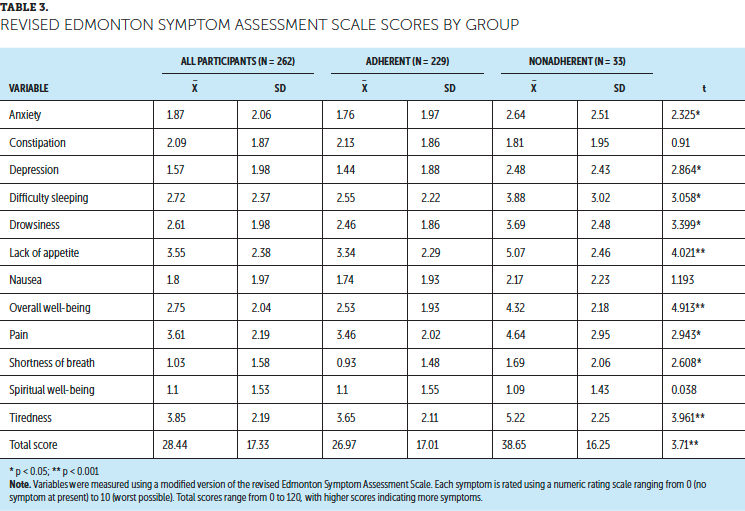
Aim 4: Neither spirituality nor pain levels were associated with number of reflexology sessions completed during each time interval (weeks 2–5 and weeks 6–11) when considering demographic and clinical factors. The interactions between pain and spirituality were also not significant at either time point and, thereby, were not reported. In weeks 6–11, participants identifying as Christian (versus non-Christian) and those receiving chemotherapy or targeted therapy (versus hormonal therapy) had slightly higher odds of completing more reflexology sessions (see Table 4). 
Discussion
Women with advanced breast cancer experience a significant level of pain (Flanigan et al., 2019; Perroud et al., 2016), which was confirmed by this study. Using previously validated cut points (Given et al., 2008), these women experienced moderate pain, which can significantly contribute to QOL (Rodriguez et al., 2019) and can result in cancer treatment dose delays and interruptions (Wyatt et al., 2015). These findings underscore the need for additional support for comprehensive pain management in this population.
Findings revealed that various demographic and clinical factors, including age, marital status, employment status, and treatment type, were associated with pain in this sample. Previous studies have shown mixed results on the association between age and pain, which partially support the finding that younger women with advanced breast cancer may experience greater pain than older women. One study reported significant differences in pain level across age groups, with younger adults experiencing more pain (Stuver et al., 2012), and another found variation in pain intensity descriptions based on age (Gauthier et al., 2018). However, other work has reported no correlation between age and pain (Sanford et al., 2019). Two previous studies reported significant associations between marital status and pain (Aneja & Yu, 2016; Posternak et al., 2016). Prior research also supported the association between employment status and pain (Posternak et al., 2016). Although no research was identified that examined relationships between treatment type and pain in individuals with advanced cancer, this work found that women receiving hormonal therapy had slightly higher odds of pain. This may be because of the high incidence of joint and bone pain associated with the use of aromatase inhibitors among women with advanced breast cancer (Nyrop et al., 2016).
Multiple demographic and clinical factors were also associated with spirituality, including age, race, and religious preference. The association between age and self-reported spirituality is supported by one previous study that yielded similar findings, suggesting that spiritual aspects of life become more salient with increased age (Mystakidou et al., 2008). The finding that women identifying as non-White had increased odds of a higher spirituality level was also aligned with previous findings. Studies have indicated that African Americans with cancer place particularly high value on spirituality in advanced illness (Bai et al., 2018; Gaston-Johansson et al., 2013). Other studies have found that the highest percentage of women with breast cancer identifying as spiritual were Asian/Pacific Islanders (Levine et al., 2007), and that Asian American breast cancer survivors were more likely to engage in spiritual practices compared to White survivors (Levine et al., 2009). The finding that women identifying as religious had increased odds of having a higher level of spirituality is partially supported by prior studies (Gaston-Johansson et al., 2013). Studies support the idea that religion and spirituality are distinct but related concepts (Lazenby, 2018) and that involvement with religion can strengthen aspects of spirituality, such as connection to others and connection with a higher power (Sherman et al., 2015).
Self-reported spirituality was not found to alter pain in this sample of women with advanced breast cancer. This finding contrasts with previous studies that yielded significant relationships between pain and spirituality in various samples of individuals with cancer (Bai et al., 2018; Delgado-Guay et al., 2016; Wang & Lin, 2016). This null finding could have been a result of the particularly high level of self-reported spirituality within this sample (mean = 3.2 of 4) and, thereby, little variation in spirituality levels. Previous studies found that higher self-reported spirituality may be associated with greater openness toward CIH therapies (Smith et al., 2008). Because of the nature of the parent study (a CIH intervention, reflexology), women with higher spirituality may have been more likely to enroll than those with lower spirituality. Therefore, the women enrolled in this study may have important differences compared to the entire population of women with advanced breast cancer. Because enrollment in the CIH trial may have influenced results, future research examining spirituality level and contribution of spirituality to pain experiences in a sample representative of the overall population of women with advanced breast cancer may provide additional insights.
Spirituality did not alter the uptake of the CIH self-management intervention. This finding is in contrast to previous studies that suggest that higher self-reported spirituality is related to higher use of self-management interventions (Harvey, 2008; Yeager et al., 2016; Zarei et al., 2015). Because the intervention was caregiver-delivered, women were reliant on caregivers to complete their sessions. Therefore, various caregiver characteristics or relationship dynamics could have contributed to intervention engagement. Understanding the factors associated with intervention engagement could help predict which individuals are most likely to be successful with various interventions. For example, previous work has identified that expectations related to the success of CIH interventions may influence intervention engagement (Rottman et al., 2020). Research exploring additional characteristics in relation to intervention engagement is warranted.
Limitations
This study has some limitations to note. The sample had low diversity across various demographic markers. This sample of women was primarily White (83%) and fairly well educated (76% had some college education), and a majority were married (69%). Because the sample was very homogenous and all women were enrolled in a CIH intervention trial, findings may not be generalizable to other populations. In addition, although the PROMIS items are well tested (HealthMeasures, 2018), a one-item pain measure may not be optimal when examining this complex concept, so specific intricacies of women’s pain experiences (such as pain interference and unpleasantness) may have been missed. Because this was a secondary analysis, available measurements were limited. Future research can account for this limitation by using more comprehensive instruments that can examine the complexities of pain. Specific types of pain (e.g., acute, chronic, somatic, visceral, neuropathic) were not assessed and should be considered in future work. Finally, the use of a lay caregiver–delivered intervention to examine spirituality’s effect on intervention engagement is less ideal for a study of this nature. In the parent study, the women with advanced breast cancer likely had a high degree of control over practicing reflexology, but unable to be accounted for was the effect of the caregiver’s willingness to engage in the intervention. Despite these limitations, this work contributes novel insights that may be used to enhance nursing care for women with advanced breast cancer.
Implications for Nursing
These findings provide one of the first examinations of the contribution of spirituality to experiences of pain among women with advanced breast cancer. Nurses are in a unique position to enhance pain management strategies and support spirituality for individuals with advanced cancer through CIH approaches (Blackburn et al., 2019; Moosavi et al., 2019). In this study, information on which subpopulations of women are most at risk for issues with pain and spirituality were revealed, which can affect nursing practice and research. Oncology nurses can identify women who may be in need of additional support with pain management to provide individualized interventions. Nurse researchers can use this information to control for important demographic and clinical factors in future studies and to develop targeted interventions for subgroups of women. Although no significant relationship between level of self-reported spirituality and pain was found, this study underscores the need for enhanced pain management for women with advanced breast cancer. This sample of women had moderate pain, on average, indicating a need for enhanced pain management. Clinical nurses could be well served to conduct comprehensive assessments of pain and employ basic nonpharmacologic pain interventions when possible (Blackburn et al., 2019; Eaton et al., 2017). Further understanding of cognitive and emotional aspects of pain in women with advanced breast cancer could be a promising avenue for advancing nursing science (Brown et al., 2020). Future research is needed that focuses on developing nurse-led pain management interventions, with mechanisms targeting cognitive and emotional routes, possibly including spirituality. These novel interventions may include components of mindfulness meditation (Wren et al., 2019), yoga (Carson et al., 2017), prayer (Eilami et al., 2019), and art making (Kim et al., 2018). Because pain and spirituality are significant aspects of the advanced breast cancer experience, oncology nurses are urged to holistically manage pain and support spirituality with these women. 
Conclusion
Despite significant advancements in care, this sample of women with advanced breast cancer reported experiencing moderate pain, on average. Multiple demographic and clinical factors were found to be associated with higher pain level (younger age, not married or partnered, not employed, receiving hormonal therapy) and lower spirituality level (younger age, non-White race, non-Christian religious preference). These results indicate that some subgroups of women may require additional support, particularly with pain management. Level of self-reported spirituality did not contribute to the level of pain in this sample of women. This null finding could have been because of ceiling effects and little variation in spirituality level across participants; therefore, further investigation is needed. Self-reported spirituality and pain were not associated with uptake of the reflexology intervention, indicating a need for further research into potential factors contributing to intervention engagement. Overall, this work highlights the need for continued nursing efforts to enhance pain management strategies for individuals with advanced cancer, which may include components of spirituality.
About the Author(s)
Megan Miller, PhD, RN, is a PhD candidate and graduate teaching assistant in the College of Nursing at Michigan State University in East Lansing; Ding Xu, MS, BS, is a data scientist at Shanghai Pudong Development Bank in China; and Rebecca Lehto, PhD, RN, FAAN, is an associate professor in the College of Nursing, Jason Moser, PhD, is an associate professor in the Department of Psychology, and Horng-Shiuann Wu, PhD, RN, is an associate professor and Gwen Wyatt, PhD, RN, FAAN, is a professor, both in the College of Nursing, all at Michigan State University. This work was supported by the Virginia Kelly Fund of the American Nurses Foundation, the Blue Cross Blue Shield of Michigan Foundation, and the National Cancer Institute (5R01CA157459). Lehto, Moser, Wu, and Wyatt contributed to the conceptualization and design. Miller and Wyatt completed the data collection. Moser provided statistical support. Miller, Xu, Moser, and Wyatt provided the analysis. Miller, Lehto, Moser, Wu, and Wyatt contributed to the manuscript preparation. Miller can be reached at miller89@wisc.edu, with copy to ONFEditor@ons.org. (Submitted March 2020. Accepted June 25, 2020.)




