Weight Management: Perception, Interest, and Preferences in Adult Cancer Survivors
Background: Obesity in cancer survivors has been recognized as a growing crisis in cancer care, but cancer survivors may not perceive weight status as important and may not be motivated to manage weight.
Objectives: This study aims to evaluate survivors’ perception, interest, and preferences for weight management and to identify characteristics that may affect attitudes toward weight management.
Methods: This cross-sectional survey assessed cancer survivors’ attitudes toward weight management with patients attending oncology outpatient clinics at Tufts Medical Center in Boston, Massachusetts.
Findings: Among 209 respondents who completed the survey, 35% were overweight and 27% were obese. Most participants indicated that they would like to lose weight or were interested or very interested in participating in weight management programs. The results reinforce the need for the oncology team to provide weight management support to cancer survivors.
Jump to a section
With advancements in cancer screening and treatment, cancer mortality rates continue to decline for most major cancer types in the United States (Lerro, Stein, Smith, & Virgo, 2014), which translates to a growing cohort of cancer survivors, defined as any individuals with a diagnosis of cancer (Bell & Ristovski-Slijepcevic, 2013). However, this success has also brought the recognition that cancer survivors have elevated prevalence of comorbidities, such as diabetes, congestive heart failure, and cerebrovascular diseases (Edwards et al., 2013). Comorbidities are important predictors for mortality and, consequently, the overall survival of patients with cancer (Edwards et al., 2013).
Obesity is a known risk factor for many chronic health conditions and a recognized risk factor for several cancers. A high proportion of patients with cancer are overweight or obese at diagnosis, and many continue to gain weight after diagnosis (Vance, Mourtzakis, McCargar, & Hanning, 2011). Obesity at diagnosis and undesirable weight gain postdiagnosis contribute to an elevated risk of chronic health conditions in cancer survivors (Demark-Wahnefried et al., 2012; Nichols et al., 2009), and, for many cancer types, obesity and weight gain are also associated with poor survival outcomes, such as cancer recurrence and death (Kroenke, Chen, Rosner, & Holmes, 2005; Protani, Coory, & Martin, 2010). In addition, obesity can interfere with effective delivery of cancer treatment and contribute to treatment failure (Rock & Demark-Wahnefried, 2002).
In 2012, the American Cancer Society published the first nutrition and physical activity guidelines for cancer survivors, recommending that cancer survivors achieve and maintain a healthy weight (Rock et al., 2012). However, the level of interest in weight management programs and perception of weight management as important for cancer survivors remains unclear. The primary purposes of this study are (a) to evaluate cancer survivors’ perception, interest, and preferences for weight management and (b) to identify patient and treatment characteristics that may affect survivors’ attitudes toward weight management. This understanding is critical to the development of individualized and comprehensive plans for survivorship care.
Methods
From August to October 2012, patients aged 18 years or older who attended the oncology outpatient clinics at Tufts Medical Center in Boston, Massachusetts, were given an anonymous survey to complete. Survey questionnaires were placed in a folder at the reception desk, and patients were told that survey completion was voluntary and that their choice of participation would not affect their clinical care. Survivors were asked to deposit the completed survey in a designated collection box placed in the clinic’s waiting room. The anonymous survey was first conducted in the breast health clinic and the hematology/oncology clinic during the first two months and was expanded to include all oncology clinics in the last month. The study was granted a waiver of document of consent. The institutional review board at Tufts Medical Center approved this study.
Survey Instrument
The self-administered survey included 32 items about patient and treatment characteristics and thoughts about weight status, as well as beliefs about, interest in, and preference for weight management. Participants were asked about their age, gender, current weight and height, type of cancer diagnosed, age at diagnosis, and treatment status. Those who had completed treatment were asked how long ago the last treatment was. Participants were then asked to choose the best answer to describe their thoughts about current weight status from one of the four choices: (a) I would like to gain weight, (b) I would like to stay at my current weight, (c) I would like to lose weight, and (d) I do not think about my weight. The survey also measured agreement using responses of “yes” or “no” on certain attitudes or beliefs about weight status and weight management, such as “I believe being overweight or obese could cause my cancer to come back,” “I believe being overweight or obese affects my overall health,” “I believe being a little overweight can help me battle against cancer,” “I have always tried to be at a healthy weight,” and “weight management is not a priority for me as a patient with cancer or survivor.” Participants were asked to rate their interest in participating in weight management programs using a four-point Likert-type scale from 1 (not at all interested) to 4 (very interested). Participants who indicated any level of interest were asked to indicate optimal timing for participating in weight management programs: (a) after diagnosis and before treatment completion, (b) right after treatment completion, (c) at least one year after treatment completion, (d) at least five years after treatment completion, or (e) any time. They were also asked to indicate whether or not they were interested in participating in five common types of weight management activities (i.e., nutrition counseling, cooking demonstrations, discussions about weight and cancer, aerobic exercise, or strength training), location (i.e., cancer clinic, community center, or home), intensity (i.e., a few times a week, once a week, or less than once a week), and with whom they would like to participate (i.e., other cancer survivors, family members, friends, or alone).
The survey items were developed by the current authors for the purpose of the study. To ensure face validity, an oncologist (JE), an oncology nurse (MS), and a survey expert (SK) were asked to review the survey items and give their opinions on the relevance of the questions. Per their feedback, certain questions were clarified, including simplifying items on optimal timing and intensity. In addition, three-point Likert-type scales from 1 (not interested) to 3 (interested) were added to assess levels of interest on the following items: type of weight management activities, location, intensity, and with whom respondents would like to participate. After the modifications were made, the survey reviewers reported that the survey instrument was easy to comprehend and measured the aspects of cancer survivors’ attitudes toward weight management that it intended to measure.
Statistical Analysis
Descriptive analyses were performed on participants’ demographic and treatment characteristics, thoughts on current weight status, and levels of interest in participating in weight management programs using mean and standard deviation for continuous variables and n values for categorical variables. Comparisons were made between participants who indicated that they would like to lose weight to those who indicated they would like to maintain or gain weight for differences in patient and treatment characteristics using analysis of variance (ANOVA) for continuous variables and chi-square tests for categorical variables. Multivariate logistic regression models were performed to evaluate patient and treatment characteristics in association with thoughts on current weight status by simultaneously adjusting for variables that showed significant differences in the univariate analyses.
Differences in patient and treatment characteristics by level of interest in participating in weight management programs were also analyzed. Participants were initially categorized into four groups (1 = not interested, 2 = a little interested, 3 = interested, 4 = very interested). However, because of limited sample size, “interested” or “very interested” participants were combined into a single group. The differences in patient and treatment characteristics by levels of interest were analyzed using ANOVA for continuous variables and chi-square tests for categorical variables. A multinomial logistic regression model was performed to evaluate associations between patient and treatment characteristics and interest in weight management by comparing participants who were interested or very interested and those who were a little interested to a common reference group (i.e., participants who were not at all interested), and simultaneously adjusted for variables that showed significant difference in the univariate analyses. Among participants who indicated any level of interest in participating in weight management programs, the frequencies were summarized for participants’ preferences in timing, program activity type, location, intensity, and people with whom they would like to participate. All statistical tests were two-sided with a type I error of 0.05 and were performed using SAS®, version 9.3.
Results
Two hundred and twenty-two patients responded to the survey. Eight did not report a diagnosis of cancer, and five did not answer 80% or more of the survey questions and were excluded from the analyses. In the remaining 209 surveys, the mean age of the respondents was 58.3 years (SD = 11.3, range = 28–89). The majority of the respondents were female. The average body mass index (BMI) was 27.9 kg/m2 (SD = 6.2). None were underweight (BMI less than 18.5 kg/m2), 35% (n = 69) were overweight (BMI = 25-29.9 kg/m2), and 27% (n = 54) were obese (BMI of 30 kg/m2 or greater). The most common primary cancer diagnosis was breast cancer, followed by hematologic cancers and other cancer types. The mean time since diagnosis was 7.3 years (SD = 7.2, range = 0–32). Eighty-five respondents were still undergoing treatment at the time of survey completion. Among the 117 respondents who were done with treatment, 63 were within five years post-treatment completion, and 54 were more than five years post-treatment completion (see Table 1).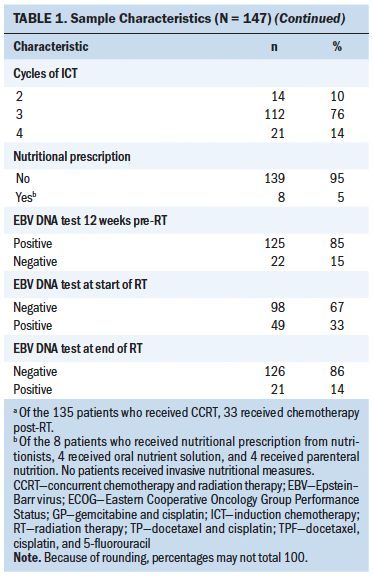
More than half of the respondents indicated that they would like to lose weight. Compared to those who would like to gain or maintain weight (n = 72), respondents who wanted to lose weight were younger (aged 56.2 years versus 61.1 years, p = 0.003), weighed more (BMI of 30.2 kg/m2 versus 24.2 kg/m2, p < 0.0001), were more likely to be overweight or obese (78% versus 36%, p < 0.0001), and had completed treatment at least five years ago (31% versus 19%, p = 0.04). In multivariate logistic regression model that simultaneously adjusted for age, weight status, and treatment status, age was inversely associated with thoughts toward weight loss (odds ratio [OR] = 0.8, 95% confidence interval [CI] [0.6, 0.9]). Respondents who wanted to lose weight were three times more likely to have completed treatment at least five years ago (OR = 3.3, 95% CI [1.3, 8.5]) and eight times more likely to be overweight or obese (OR = 8.1, 95% CI [3.8, 17.3]) than those who wanted to maintain or gain weight. Respondents did not differ in gender, time since diagnosis, or cancer type in their thoughts about weight status.
Most participants were at least somewhat interested in weight management. Being overweight or obese was positively associated with the rating of interested or very interested (OR = 3.7, 95% CI [1.7, 8.2]), and increasing age was inversely associated with the rating of interested or very interested (for each five-year increase in age, OR = 0.8, 95% CI [0.7, 0.9]). Survivors’ interest in participating in weight management was not related to treatment status, gender, interval from diagnosis, or cancer type.
Among the 109 respondents who were interested in weight management at any level, 90% or more provided answers to questions that further inquired about their preferences on the timing (n = 98, 90%), intensity (n = 101, 93%), location (n = 107, 98%), and types of activities (n = 105, 96%) for weight management, and with whom they would like to participate in weight management (n = 106, 97%). Among those who provided answers (N = 98), about half (n = 48) indicated that they would like to join a weight management program at any time, followed by those who would like to join right after completion of cancer treatment (n = 18), at least a year after treatment completion (n = 16), after diagnosis and during treatment (n = 10), or at least five years post-treatment (n = 6). For optimal intensity of weight management (N = 101), about half (n = 48) of the respondents indicated that they would like to participate a few times a week, followed by those who would like to participate once a week (n = 39) or less than once a week (n = 14). For preference on activity type (N = 105), respondents were mostly interested in strength training (n = 85, 83%), followed by nutrition counseling (n = 83, 81%), aerobic exercise (n = 69, 71%), discussions on weight and cancer (n = 85, 62%), or cooking demonstrations (n = 54, 56%). Respondents (N = 107) were mostly interested in home- (n = 61, 68%) or community-based (n = 56, 62%) programs, and only 40% (n = 36) were interested in participating at the cancer clinics where they receive treatment and survivorship care. Respondents (N = 106) wanted to participate in weight management with other cancer survivors (n = 59, 62%), followed by family members (n = 46, 53%), themselves (n = 43, 51%), or friends (n = 39, 46%).
Discussion
Obesity in cancer survivors has been recognized as a growing crisis in cancer care (Ligibel et al., 2014), but cancer survivors’ attitudes toward weight management have not been formally evaluated. In this cross-sectional survey of 209 adult cancer survivors, more than half of the survivors indicated that they would like to lose weight, and about one-third were interested or very interested in participating in weight management following cancer diagnosis and treatment. In addition, age and weight status were significant predictors of attitudes toward weight management in this population of adult cancer survivors. These findings provide further insight into the growing body of literature on weight-related concerns in cancer survivors.
An increasing body of evidence suggests that obesity at or after cancer diagnosis is associated with an increased risk for cancer recurrence and mortality, particularly for women diagnosed with breast cancer (Demark-Wahnefried et al., 2015; World Cancer Research Fund International, 2014). A meta-analysis that analyzed weight status and survival in 213,075 breast cancer survivors across 82 studies identified a 14%–29% increased risk of cancer-specific mortality and an 8%–17% increased risk of all-cause mortality associated with each 5 kg/m2 increment in BMI (Chan et al., 2014). Similar associations were observed for other major cancer types, such as colorectal and prostate cancers (Cao & Ma, 2011; Wu et al., 2014). Although survivors who are underweight also experience poor survival outcomes (Demark-Wahnefried et al., 2015), a large proportion of cancer survivors are overweight or obese at the time of diagnosis, and many experience undesirable weight gain after diagnosis and treatment. For example, undesirable weight gain is reported in breast cancer survivors receiving adjuvant chemotherapy (Demark-Wahnefried et al., 2001) and prostate cancer survivors receiving androgen-deprivation therapy (Haseen, Murray, Cardwell, O’Sullivan, & Cantwell, 2010). As many as 50%–96% of breast cancer survivors experience weight gain during treatment, ranging, on average, from 2.5–6.2 kg (Vance et al., 2011). Many, including those whose weight remains stable during treatment, report progressive weight gain in the months and years after treatment (Vance et al., 2011).
Although the importance of maintaining a healthy weight for cancer survivors has been increasingly recognized by cancer care providers (Ligibel et al., 2014), cancer survivors themselves may not perceive weight management as a health priority after surviving a life-threatening event. Alternatively, cancer diagnosis may serve as a teachable moment and spur cancer survivors to make positive behavioral changes related to their health (Demark-Wahnefried, Aziz, Rowland, & Pinto, 2005). In the American Cancer Society Studies of Cancer Survivors II, 35% of cancer survivors reported they attempted to lose weight (Blanchard, Courneya, & Stein, 2008). In the current sample of adult cancer survivors, more than half indicated they would like to lose weight, and 22% were interested and 10% were very interested in participating in weight management programs. Many survivors linked obesity to general health, but fewer related it to survival. For example, 76% of the survivors believe that being overweight or obese affects their overall health, and 36% believe being overweight or obese can cause cancer to come back. Increasing evidence links obesity to elevated risk of recurrence and cancer-related mortality (Ligibel et al., 2014). This evidence calls for future interventions to improve survivors’ knowledge of weight status and long-term health, particularly for those diagnosed with early-stage disease.
In the current sample, being overweight or obese was the most significant predictor for survivors’ attitudes toward weight management. However, among survivors who were overweight or obese, about 25% indicated weight management was not a priority. Younger survivors were more likely to express interest in joining weight management programs than older survivors, consistent with findings from a previous study that also showed higher levels of interest in health promotion in younger survivors (Demark-Wahnefried, Peterson, McBride, Lipkus, & Clipp, 2000). These results are promising, given that younger survivors have long life expectancies and that weight management can have a significant effect on quality of life. In the current study, attitudes toward weight management did not differ in male versus female survivors. However, the majority (86%) of survivors who completed the survey were women, and, therefore, gender comparisons were limited by statistical power. Future studies should explore potential gender differences in attitudes toward weight management. Cancer survivors may attempt to make positive behavioral changes soon after diagnosis (Blanchard et al., 2003; Humpel, Magee, & Jones, 2007; Maunsell, Drolet, Brisson, Robert, & Deschenes, 2002; Patterson et al., 2003; Thomson et al., 2002), but existing evidence suggests that their long-term health behaviors and weight status are not necessarily better than those of the general population (Bellizzi, Rowland, Jeffery, & McNeel, 2005; Courneya, Katzmarzyk, & Bacon, 2008; Milliron, Vitolins, & Tooze, 2014).
This study did not find time since diagnosis to be associated with attitudes toward weight management. Although survivors who had completed treatment at least five years ago were more likely to think about weight loss than survivors who were still undergoing treatment, all showed similar levels of interest in participating in weight management programs. The leading response for the time preference for initiating weight management was right after completion of cancer treatment. However, the findings in this study show that waiting too far beyond completion of cancer treatment may not be beneficial because interest level may decline over time. Only 6% of the survivors who were interested in weight management considered initiating the program at least five years post-treatment. The authors did not find that attitudes toward weight management differed by cancer type. Although the majority of survivors in this study were breast cancer survivors, the ability to explore this question was limited. Future studies involving a large heterogeneous group of cancer survivors are needed to further evaluate whether attitudes toward weight management differ by cancer type.
As expected, dietary counseling is a component in weight management that interested many survivors. This study indicates that cancer survivors have particularly poor adherence to nutritional guidelines in a number of areas, such as high consumption of empty calories (calories from added sugars and solid fats) and sodium and low consumption of dietary fiber (Zhang, Liu, John, Must, & Demark-Wahnefried, 2015). Many of the existing weight management programs for cancer survivors focused exclusively on exercise, with only a few targeting dietary modification (either diet alone or diet combined with physical activity component) (Demark-Wahnefried et al., 2015; Playdon et al., 2013). For obesity prevention, dietary modification to reduce caloric intake on a daily basis is essential to achieve energy balance, and the same amount of calorie reduction can be more readily achieved by cutting one can of sugar-sweetened beverage (i.e., 150 calories) than by adding brisk walking for 30 minutes per day. However, cancer survivors can experience loss of lean mass as a result of cancer treatment (Demark-Wahnefried et al., 2001; Sheean, Hoskins, & Stolley, 2012), and weight management programs focusing on diet alone could lead to sarcopenic obesity. In this study, the largest proportion of survivors were interested in strength training as a weight management component, followed by dietary counseling and aerobic exercise. Many survivors were also interested in discussions on weight and cancer. Taken together, these findings suggest that future interventions could incorporate diet counseling and exercise (particularly strength training), include discussions on how survivors’ weight status affects their long-term health, and be delivered at home or in community settings. Future programs should also consider peer group interventions because the highest proportion of the survivors preferred joining with other survivors.
Strengths and Limitations
This study represents one of the first efforts to assess attitudes toward weight management in cancer survivors, but limitations exist. The survey respondents came from a convenience sample of cancer survivors attending oncology clinics during a limited period of time. The majority of the cancer survivors who completed the survey were women diagnosed with breast cancer, which limits the generalizability of the findings to other cancer types, as well as formal evaluation on survivors’ attitudes by different cancer types. Cancer survivors who are underweight may possess different attitudes toward weight management compared those who have normal weight or are overweight or obese. None of the survivors included in this study had BMI of less than 18.5 kg/m2. Therefore, the findings cannot apply to survivors who are underweight. In addition, survivors’ weight status was based on self-report, which may result in misclassification bias. Although it is reasonable to suspect that survivors who responded to the survey are more likely to be health conscious than those who did not respond, data were not collected on survivors who chose not to complete the survey, so the authors could not formally assess the possibility of response bias. In addition, the survey conducted at a single institution may compromise the generalizability of the findings to other cancer survivors. Finally, the survey did not ask survivors’ racial or ethnic background, education, and income. Therefore, the authors could not evaluate whether attitudes toward weight management differ by race and socioeconomic status. Because of the heterogeneity in cancer treatments and tumor characteristics associated with different cancer diagnoses, the authors did not collect information on the type of cancer treatment and tumor stage and were not able to evaluate whether attitudes toward weight management differ by treatment and tumor characteristics.
Implications for Practice
Because of frequent interactions with patients with cancer, oncology nurses have the potential to play a key role in increasing awareness for the importance of weight management. The findings from this study indicate that oncology nurses should (a) engage patients in weight management conversations as an integral part of cancer care and (b) direct survivors to credible resources for weight management. Topics may include why weight management is important to survivors’ long-term health and how cancer treatments may affect survivors’ intake patterns. Topics could also include activity and weight status and existing nutrition and physical activity guidelines, such as the American Cancer Society’s Nutrition and Physical Activity Guidelines for Cancer Survivors (Kushi et al., 2012), the World Cancer Research Foundation and American Institute for Cancer Research (2007) nutrition recommendations, and the 2015–2020 Dietary Guidelines for Americans (Office of Disease Prevention and Health Promotion, 2015). Cancer survivors may experience specific barriers for making healthy food choices and maintaining active living (e.g., food craving, change in taste preference, fatigue, distress), but healthcare providers can refer patients to registered dietitians who are experts in oncology care to help patients identify strategies to overcome these barriers. However, resources, such as weight management and web-based programs, are needed to provide cancer survivors with tools to address weight management. Social media could be leveraged to help deliver weight management programs through social networking sites of cancer survivors, advocates, and support groups. However, programs delivered to cancer survivors must be based on strong scientific evidence for efficacy. 
Conclusion
This study provides important evidence regarding attitudes toward weight status and management in adult cancer survivors. According to this study, a large proportion of adult cancer survivors want to lose weight, and many show interest in joining weight management programs, particularly younger and overweight or obese survivors. These findings reinforce the need for the oncology team to provide weight management support to cancer survivors that focus on strength training and diet counseling, preferably delivered at home or in community centers soon after completion of cancer treatment.
[[{"type":"media","view_mode":"media_original","fid":"29146","field_deltas":{"1":{}},"link_text":null,"fields":{},"attributes":{"height":"507","width":"366","class":"media-image media-element file-media-original","data-delta":"1"}}]]
About the Author(s)
Fang Fang Zhang, MD, PhD, is an assistant professor in the Department of Nutrition Science in the Friedman School of Nutrition Science and Policy; and Susan Meagher, PhD, is a psychologist in the Department of Psychiatry, and Susan Koch-Weser, PhD, ScD, is an assistant professor in the Department of Public Health, both in the School of Medicine, all at Tufts University in Boston, MA; Mary Beth Singer, MS, ANP-BC, AOCN®, ACHPN, is an oncology nurse practitioner at the Tufts Medical Center Cancer Center in Boston; Geetika Dhaundiyal, MS, is an operations lead at Accretive Health, Inc., in Chicago, IL; John Erban, MD, is the clinical director at the Tufts Medical Center Cancer Center; and Edward Saltzman, MD, is an associate professor in the Department of Nutrition Science in the Friedman School of Nutrition Science and Policy at Tufts University. Zhang can be reached at fang_fang.zhang@tufts.edu, with copy to CJONEditor@ons.org. (Submitted November 2015. Accepted April 13, 2016.). The authors take full responsibility for this content. This study was supported by grants from the Boston Nutrition Obesity Research Center (P30DK46200), the National Center for Research Resources (UL1 RR025752), the National Center for Advancing Translational Sciences and the National Institutes of Health (UL1 TR000073), and by a Tufts Collaborates grant. The article has been reviewed by independent peer reviewers to ensure that it is objective and free from bias.
References
Bell, K., & Ristovski-Slijepcevic, S. (2013). Cancer survivorship: Why labels matter. Journal of Clinical Oncology, 31, 409–411. doi:10.1200/jco.2012.43.5891
Bellizzi, K.M., Rowland, J.H., Jeffery, D.D., & McNeel, T. (2005). Health behaviors of cancer survivors: Examining opportunities for cancer control intervention. Journal of Clinical Oncology, 23, 8884–8893. doi:10.1200/jco.2005.02.2343
Blanchard, C.M., Courneya, K.S., & Stein, K. (2008). Cancer survivors’ adherence to lifestyle behavior recommendations and associations with health-related quality of life: Results from the American Cancer Society’s SCS-II. Journal of Clinical Oncology, 26, 2198–2204. doi:10.1200/jco.2007.14.6217
Blanchard, C.M., Denniston, M.M., Baker, F., Ainsworth, S.R., Courneya, K.S., Hann, D.M., . . . Kennedy, J.S. (2003). Do adults change their lifestyle behaviors after a cancer diagnosis? American Journal of Health Behavior, 27, 246–256.
Cao, Y., & Ma, J. (2011). Body mass index, prostate cancer-specific mortality, and biochemical recurrence: A systematic review and meta-analysis. Cancer Prevention Research, 4, 486–501. doi:10.1158/1940-6207.capr-10-0229
Chan, D.S., Vieira, A.R., Aune, D., Bandera, E.V., Greenwood, D.C., McTiernan, A., . . . Norat, T. (2014). Body mass index and survival in women with breast cancer-systematic literature review and meta-analysis of 82 follow-up studies. Annals of Oncology, 25, 1901–1914.
Courneya, K.S., Katzmarzyk, P.T., & Bacon, E. (2008). Physical activity and obesity in Canadian cancer survivors: Population-based estimates from the 2005 Canadian Community Health Survey. Cancer, 112, 2475–2482. doi:10.1002/cncr.23455
Demark-Wahnefried, W., Aziz, N.M., Rowland, J.H., & Pinto, B.M. (2005). Riding the crest of the teachable moment: Promoting long-term health after the diagnosis of cancer. Journal of Clinical Oncology, 23, 5814–5830. doi:10.1200/jco.2005.01.230
Demark-Wahnefried, W., Peterson, B., McBride, C., Lipkus, I., & Clipp, E. (2000). Current health behaviors and readiness to pursue life-style changes among men and women diagnosed with early stage prostate and breast carcinomas. Cancer, 88, 674–684.
Demark-Wahnefried, W., Peterson, B.L., Winer, E.P., Marks, L., Aziz, N., Marcom, P.K., . . . Rimer, B.K. (2001). Changes in weight, body composition, and factors influencing energy balance among premenopausal breast cancer patients receiving adjuvant chemotherapy. Journal of Clinical Oncology, 19, 2381–2389.
Demark-Wahnefried, W., Platz, E.A., Ligibel, J.A., Blair, C.K., Courneya, K.S., Meyerhardt, J.A., . . . Goodwin, P.J. (2012). The role of obesity in cancer survival and recurrence. Cancer Epidemiology, Biomarkers, and Prevention, 21, 1244–1259. doi:10.1158/1055-9965.epi-12-0485
Demark-Wahnefried, W., Rogers, L.Q., Alfano, C.M., Thomson, C.A., Courneya, K.S., Meyerhardt, J.A., . . . Ligibel, J.A. (2015). Practical clinical interventions for diet, physical activity, and weight control in cancer survivors. CA: A Cancer Journal for Clinicians, 65, 167–189.
Edwards, B.K., Noone, A.-M., Mariotto, A.B., Simard, E.P., Boscoe, F.P., Henley, S.J., . . . Ward, E.M. (2013). Annual report to the nation on the status of cancer, 1975–2010, featuring prevalence of comorbidity and impact on survival among persons with lung, colorectal, breast, or prostate cancer. Cancer, 120, 1290–1314. doi:10.1002/cncr.28509
Haseen, F., Murray, L.J., Cardwell, C.R., O’Sullivan, J.M., & Cantwell, M.M. (2010). The effect of androgen deprivation therapy on body composition in men with prostate cancer: Systematic review and meta-analysis. Journal of Cancer Survivorship, 4, 128–139. doi:10.1007/s11764-009-0114-1
Humpel, N., Magee, C., & Jones, S.C. (2007). The impact of a cancer diagnosis on the health behaviors of cancer survivors and their family and friends. Supportive Care in Cancer, 15, 621–630. doi:10.1007/s00520-006-0207-6
Kroenke, C.H., Chen, W.Y., Rosner, B., & Holmes, M.D. (2005). Weight, weight gain, and survival after breast cancer diagnosis. Journal of Clinical Oncology, 23, 1370–1378.
Kushi, L.H., Doyle, C., McCullough, M., Rock, C.L., Demark-Wahnefried, W., Bandera, E.V., . . . Gansler, T. (2012). American Cancer Society guidelines on nutrition and physical activity for cancer prevention: Reducing the risk of cancer with healthy food choices and physical activity. CA: A Cancer Journal for Clinicians, 62, 30–67. doi:10.3322/caac.20140
Lerro, C.C., Stein, K.D., Smith, T., & Virgo, K.S. (2014). A systematic review of large-scale surveys of cancer survivors conducted in North America, 2000–2011. Journal of Cancer Survivorship, 6, 115–145. doi:10.1007/s11764-012-0214-1
Ligibel, J.A., Alfano, C.M., Courneya, K.S., Demark-Wahnefried, W., Burger, R.A., Chlebowski, R.T., . . . Hudis, C.A. (2014). American Society of Clinical Oncology position statement on obesity and cancer. Journal of Clinical Oncology, 32, 3568–3574. doi:10.1200/jco.2014.58.4680
Maunsell, E., Drolet, M., Brisson, J., Robert, J., & Deschenes, L. (2002). Dietary change after breast cancer: Extent, predictors, and relation with psychological distress. Journal of Clinical Oncology, 20, 1017–1025.
Milliron, B.J., Vitolins, M.Z., & Tooze, J.A. (2014). Usual dietary intake among female breast cancer survivors is not significantly different from women with no cancer history: Results of the National Health and Nutrition Examination Survey, 2003–2006. Journal of the Academy of Nutrition and Dietics, 114, 932–937. doi:10.1016/j.jand.2013.08.015
Nichols, H.B., Trentham-Dietz, A., Egan, K.M., Titus-Ernstoff, L., Holmes, M.D., Bersch, A.J., . . . Newcomb, P.A. (2009). Body mass index before and after breast cancer diagnosis: Associations with all-cause, breast cancer, and cardiovascular disease mortality. Cancer Epidemiology, Biomarkers, and Prevention, 18, 1403–1409. doi:10.1158/1055-9965.epi-08-1094
Office of Disease Prevention and Health Promotion. (2015). Dietary guidelines for Americans 2015–2020 (8th ed.). Retrieved from http://health.gov/dietaryguidelines/2015/guidelines
Patterson, R.E., Neuhouser, M.L., Hedderson, M.M., Schwartz, S.M., Standish, L.J., & Bowen, D.J. (2003). Changes in diet, physical activity, and supplement use among adults diagnosed with cancer. Journal of the American Dietic Association, 103, 323–328.
Playdon, M., Thomas, G., Sanft, T., Harrigan, M., Ligibel, J., & Irwin, M.L. (2013). Weight loss intervention for breast cancer survivors: A systematic review. Current Breast Cancer Reports, 5, 222–246.
Protani, M., Coory, M., & Martin, J.H. (2010). Effect of obesity on survival of women with breast cancer: Systematic review and meta-analysis. Breast Cancer Research and Treatment, 123, 627–635. doi:10.1007/s10549-010-0990-0
Rock, C.L., & Demark-Wahnefried, W. (2002). Nutrition and survival after the diagnosis of breast cancer: A review of the evidence. Journal of Clinical Oncology, 20, 3302–3316.
Rock, C.L., Doyle, C., Demark-Wahnefried, W., Meyerhardt, J., Courneya, K.S., Schwartz, A.L., . . . Gansler, T. (2012). Nutrition and physical activity guidelines for cancer survivors. CA: A Cancer Journal for Clinicians, 62, 242–274. doi:10.3322/caac.21142
Sheean, P.M., Hoskins, K., & Stolley, M. (2012). Body composition changes in females treated for breast cancer: A review of the evidence. Breast Cancer Research and Treatment, 135, 663–680. doi:10.1007/s10549-012-2200-8
Thomson, C.A., Flatt, S.W., Rock, C.L., Ritenbaugh, C., Newman, V., & Pierce, J.P. (2002). Increased fruit, vegetable and fiber intake and lower fat intake reported among women previously treated for invasive breast cancer. Journal of the American Dietetic Association, 102, 801–808.
Vance, V., Mourtzakis, M., McCargar, L., & Hanning, R. (2011). Weight gain in breast cancer survivors: Prevalence, pattern and health consequences. Obesity Reviews, 12, 282–294.
World Cancer Research Fund & American Institute for Cancer Research (Eds.). (2007). Food, nutrition, physical activity, and the prevention of cancer: A global perspective. Washington, DC: American Institute for Cancer Research.
World Cancer Research Fund International. (2014). Diet, nutrition, physical activity, and breast cancer survivors. Retrieved from http://bit.ly/1re3WHv
Wu, S., Liu, J., Wang, X., Li, M., Gan, Y., & Tang, Y. (2014). Association of obesity and overweight with overall survival in colorectal cancer patients: A meta-analysis of 29 studies. Cancer Causes and Control, 25, 1489–1502. doi:10.1007/s10552-014-0450-y
Zhang, F.F., Liu, S., John, E.M., Must, A., & Demark-Wahnefried, W. (2015). Diet quality of cancer survivors and noncancer individuals: Results from a national survey. Cancer, 121, 4212–4221. doi:10.1002/cncr.29488




